
Understanding Dual Diagnosis: When Mental Health and Substance Use Overlap
Dual diagnosis treatment addresses the complex reality that mental health conditions and substance use disorders (SUDs) often occur together. Treating them simultaneously is crucial for lasting recovery. This is also known as having co-occurring disorders.
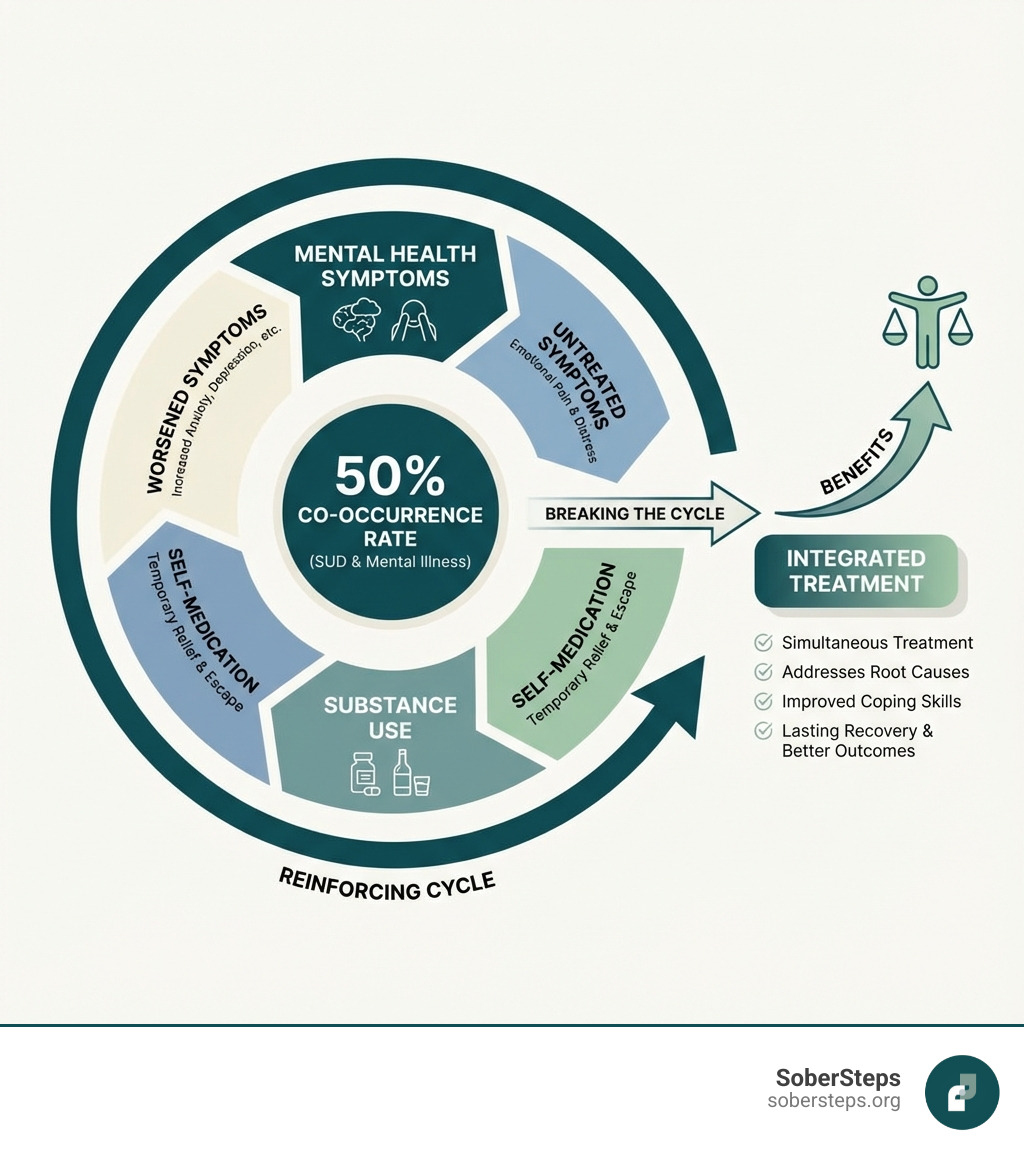
According to the Substance Abuse and Mental Health Services Administration (SAMHSA), millions of American adults experience co-occurring disorders each year. These conditions are deeply intertwined, creating a cycle where one can trigger or worsen the other. For example, a person with anxiety may use alcohol to self-medicate, but the substance use can ultimately increase their anxiety, leading to a dangerous feedback loop.
Breaking this cycle requires specialized, integrated care that addresses both issues at once. At SoberSteps, we provide resources and connections to help you find the comprehensive dual diagnosis treatment you need.
Learn more about co-occurring conditions or call our 24/7 helpline to speak with someone who understands.
What is a Dual Diagnosis?
A dual diagnosis, or co-occurring disorder, is when a person has both a mental health condition and a substance use disorder simultaneously. These conditions influence each other, making treatment more complex than addressing either one alone.
Common combinations include:
- Depression and Alcohol Use Disorder: Using alcohol to numb emotional pain, which in turn deepens depression. Learn more about Dual Diagnosis: Depression.
- Anxiety and Prescription Medication Misuse: Misusing sedatives like Xanax to manage anxiety, leading to dependence and rebound anxiety. Explore Dual Diagnosis: Anxiety.
- PTSD and Opioid Use Disorder: Using opioids to cope with trauma symptoms, which can create a new cycle of suffering. Understand Dual Diagnosis: PTSD.
- Bipolar Disorder and Alcoholism: Attempting to self-medicate mood swings with alcohol, which often exacerbates the disorder. Read about Dual Diagnosis: Bipolar Disorder.
Why Do Mental Health and Substance Use Disorders Occur Together?
The link between mental health and substance use is not a coincidence. Key reasons include:
- Shared Risk Factors: Genetic predispositions, chronic stress, and a history of trauma can increase the risk for both mental illness and addiction.
- Self-Medication: Many people use drugs or alcohol to cope with the symptoms of an undiagnosed or untreated mental health condition. While this may provide temporary relief, it almost always worsens the underlying issue over time.
- Substance Use and Brain Chemistry: Prolonged substance use can alter brain structure and function, which can trigger or worsen mental health disorders in vulnerable individuals. For example, chronic marijuana use has been linked to an increased risk of psychosis.
This vicious cycle is why integrated dual diagnosis treatment is so critical. If you’re struggling, specialized help is available. Find help for co-occurring disorders by reaching out to us today.
The Gold Standard: Integrated Dual Diagnosis Treatment Models

For co-occurring disorders, integrated dual diagnosis treatment is the gold standard of care. This approach treats both the mental health condition and the substance use disorder simultaneously, with one cohesive team and a single treatment plan. It is far more effective than outdated models like sequential treatment (treating one disorder, then the other) or parallel treatment (treating both at the same time but with separate providers).
This integrated philosophy is supported by the “no wrong door” policy, which ensures that anyone seeking help for either a mental health or substance use issue is screened for both and guided to the appropriate comprehensive care. If you or a loved one are navigating these challenges, choosing an integrated program offers the best chance for lasting recovery. Call our 24/7 helpline for treatment options and let us guide you.
The Importance and Benefits of Integrated Treatment
Integrated dual diagnosis treatment is an evidence-based approach that treats the whole person, not just isolated symptoms. The benefits are significant:
- Improved Psychiatric Symptoms: Research shows integrated care leads to superior reductions in symptoms of depression, anxiety, and PTSD.
- Reduced Substance Use: By addressing the underlying mental health triggers, individuals are better equipped to achieve and maintain sobriety.
- Better Long-Term Outcomes: This comprehensive approach reduces the risk of relapse and improves overall quality of life, including housing stability and decreased hospitalization rates.
- Coordinated Care: A single, collaborative team of professionals ensures a consistent and unified treatment plan, eliminating confusion and conflicting advice.
What are the main types of dual diagnosis treatment?
Effective dual diagnosis treatment is always integrated, but it can be delivered through various levels of care and therapeutic methods to meet individual needs.
- Therapeutic Modalities: The foundation of treatment includes evidence-based therapies like Cognitive Behavioral Therapy (CBT) and Dialectical Behavior Therapy (DBT), which help individuals change unhealthy thought patterns and develop coping skills.
- Medication Management: Medications are often used to manage mental health symptoms (e.g., antidepressants, mood stabilizers) and support addiction recovery (e.g., Medication-Assisted Treatment).
- Levels of Care: Treatment can range from intensive inpatient/residential programs for those needing 24/7 support to flexible outpatient programs for those transitioning back to daily life.
- Support Groups: Peer groups like Dual Recovery Anonymous (DRA) provide a vital sense of community and shared experience.
How is dual diagnosis treated effectively, and what is the importance of integrated treatment?
Effective treatment for dual diagnosis is, by definition, integrated. Treating the mental health issue and the substance use disorder at the same time is essential because they are interconnected. Addressing one without the other often leads to relapse, as the untreated condition continues to fuel the other.
An effective treatment plan includes:
- Comprehensive Assessment: To accurately diagnose both conditions and understand their interplay.
- Behavioral Therapies: Such as CBT and DBT to build coping skills.
- Medication Management: To stabilize mental health and manage cravings.
- Medical Detox: If needed, to safely manage withdrawal symptoms.
- Support Systems: Including peer groups and family involvement to build a strong foundation for recovery.
This integrated approach gives individuals the best chance at long-term success. Explore your treatment options today.
What are the benefits of integrated treatment for individuals with co-occurring disorders?
Integrated dual diagnosis treatment offers a more sustainable path to recovery. Key benefits include:
- Significant improvement in psychiatric symptoms, especially for anxiety, depression, and PTSD.
- Reduced substance use by addressing the root causes and triggers.
- Increased chance of successful, long-term recovery for both disorders.
- Improved overall quality of life, including better housing stability and fewer hospitalizations.
- A coordinated care team that provides a unified and consistent treatment experience.
What is the ‘no wrong door’ policy in the context of dual diagnosis treatment?
The ‘no wrong door’ policy is a crucial principle ensuring that individuals can access care regardless of where they first seek help. It means that any mental health service should screen for substance use, and any addiction service should screen for mental health issues. This approach prevents people from falling through the cracks of a fragmented system and ensures they are guided toward the integrated dual diagnosis treatment they need.
What are the specific therapeutic approaches used in dual diagnosis treatment, such as CBT and DBT?
Several evidence-based therapies are cornerstones of dual diagnosis treatment:
- Cognitive Behavioral Therapy (CBT): Helps individuals identify and change the negative thought patterns and behaviors that link their mental health symptoms and substance use. Learn more about CBT.
- Dialectical Behavior Therapy (DBT): Teaches skills in mindfulness, distress tolerance, and emotion regulation, which is highly effective for managing intense emotions without resorting to substances. Explore DBT options.
- Motivational Interviewing (MI): A collaborative counseling style that helps individuals resolve ambivalence and find their own internal motivation to change.
- Trauma-Informed Care: An approach that recognizes the prevalence of trauma and creates a safe, supportive environment for healing, which is vital as trauma is a common root cause of co-occurring disorders.
How can medication be used in dual diagnosis treatment?
Medication is a critical tool in an integrated dual diagnosis treatment plan. It is used to:
- Manage Mental Health Symptoms: Antidepressants, mood stabilizers, and other psychiatric medications help stabilize mood and reduce symptoms, which in turn reduces the urge to self-medicate.
- Support Addiction Recovery: Medication-Assisted Treatment (MAT) uses medications like buprenorphine or naltrexone to reduce cravings and withdrawal symptoms for opioid or alcohol use disorders.
- Facilitate Safe Detox: During medically supervised detox, medications are used to manage withdrawal safely and comfortably, providing a stable foundation to begin therapy. Learn more about Medical Detox Programs.
What role do support groups play in the recovery process for individuals with dual diagnosis?
Support groups are a vital part of long-term recovery. They offer:
- A sense of community with peers who understand the unique challenges of dual diagnosis.
- Emotional and social support, reducing feelings of isolation and shame.
- Accountability and motivation to stay engaged in recovery.
- Shared wisdom and practical coping strategies from others with lived experience.
Groups like Dual Recovery Anonymous (DRA) are specifically designed for this purpose and are a cornerstone of a strong aftercare plan. Find out how to stay sober with support.
When is inpatient care recommended for dual diagnosis?
Inpatient dual diagnosis treatment is recommended when an individual’s conditions are severe or unstable. Key reasons include:
- Acute psychiatric symptoms, such as suicidal thoughts, psychosis, or severe mania.
- Need for medically supervised detoxification from substances like alcohol, benzodiazepines, or opioids.
- A high-risk or unsupportive home environment that triggers substance use.
- Previous attempts at outpatient treatment have been unsuccessful.
Inpatient care provides a safe, structured, 24/7 environment to stabilize and begin intensive therapy. Explore our Inpatient options.
What are the goals of a dual diagnosis treatment program?
The overarching goal is holistic healing and long-term well-being. Key objectives include:
- Stabilizing both mental health and substance use symptoms.
- Achieving and maintaining sobriety.
- Developing healthy coping skills to manage stress and triggers.
- Improving overall quality of life and daily functioning.
- Creating a solid relapse prevention plan.
- Addressing underlying issues like trauma.
Learn more about Overcoming Drug Addiction and setting healthy goals.
How can one determine if they need an addiction treatment program versus a dual diagnosis program?
If you suspect a mental health condition is contributing to your substance use, a dual diagnosis treatment program is the best choice. Consider a dual diagnosis program if:
- You have a pre-existing mental health diagnosis.
- You use substances to cope with feelings like anxiety, sadness, or trauma.
- Previous addiction-only treatment has not led to lasting recovery.
The most reliable way to know is through a comprehensive professional assessment, which can accurately identify co-occurring disorders. Take our confidential assessment to understand your needs better.
What are the potential risks of recreational alcohol or marijuana use for individuals with mental health conditions?
For individuals with mental health conditions, even recreational use of alcohol or marijuana carries significant risks. These substances can:
- Worsen symptoms of depression, anxiety, bipolar disorder, or psychosis.
- Interfere with psychiatric medications, making them less effective or causing dangerous side effects.
- Mask underlying issues, delaying proper diagnosis and treatment.
- Increase the risk of developing a substance use disorder.
Due to these risks, abstinence is often the safest and most recommended approach. Learn more about Addiction and its risks.
Does entering a dual diagnosis program imply addiction?
Entering a dual diagnosis treatment program means you have been diagnosed with both a substance use disorder (SUD) and a mental health condition. The focus is not on the label of “addict,” but on treating these co-occurring medical conditions with an evidence-based, integrated approach. Seeking this type of specialized care is a sign of strength and a proactive step toward comprehensive healing. Explore our Addiction Recovery Blogs for more on this topic.
Should individuals with mental illness always abstain from alcohol or marijuana?
While the decision is personal and should be discussed with a doctor, abstinence is strongly recommended for most individuals with mental illness. The risks of worsening symptoms, interfering with medication, and undermining therapeutic progress are significant. For those in dual diagnosis treatment, abstaining from all non-prescribed, mood-altering substances provides the clearest path to stability and long-term recovery. For more information, explore our page on Addiction.
Take the First Step Towards Integrated Healing
Starting on the path of dual diagnosis treatment is a courageous act of self-care. If you are struggling with the combined challenges of mental health and substance use, know that recovery is not only possible but expected with the right support.
Finding help can feel overwhelming, but it is the most important step you can take. The journey begins with a comprehensive assessment to create a personalized dual diagnosis treatment plan that addresses your unique needs. The ‘no wrong door’ philosophy means that no matter where you start, help is available.
If you or a loved one are ready to take that first step, we are here for you. Our confidential 24/7 helpline is staffed by compassionate specialists who can guide you through your options and connect you with treatment providers who specialize in integrated care.
Call our 24/7 confidential helpline to explore your recovery options today. We’re ready to listen and help you find the path to lasting recovery.
Contact us for a free consultation to discuss how we can support you.
Ready to start your journey?
Call SoberSteps now or explore our treatment programs to take the first step toward integrated recovery.
Learn more about dual diagnosis and read our recovery stories for inspiration.



