
Understanding Medicare’s Role in Addiction Treatment
Medicare Coverage for Alcohol & Drug Rehab is available to help you or your loved one access the treatment you need. Here’s what you need to know right now:
Quick Answer:
- Yes, Medicare covers addiction treatment for alcohol and drug rehab
- Part A covers inpatient hospital stays and detox
- Part B covers outpatient services, therapy, and intensive programs
- Part D covers prescription medications for addiction treatment
- Coverage requires a doctor to certify the treatment is medically necessary
- You’ll pay deductibles and coinsurance based on your specific plan
Medicare generally covers drug and alcohol rehab, but the specifics can be confusing. Your coverage and out-of-pocket costs will depend on your state, your specific plan, and the services you need. With over 60 million people on Medicare, understanding these benefits is a critical first step toward recovery for many. The good news is that coverage is improving, with recent expansions in 2024 to include more types of addiction and mental health counselors.
At Sober Steps, we specialize in helping people steer their Medicare Coverage for Alcohol & Drug Rehab. Our team can provide clear guidance on your insurance benefits and connect you with the right treatment options.
Get Help Now if you’re ready to explore your treatment options, or continue reading to learn exactly what Medicare covers and how to access these benefits.
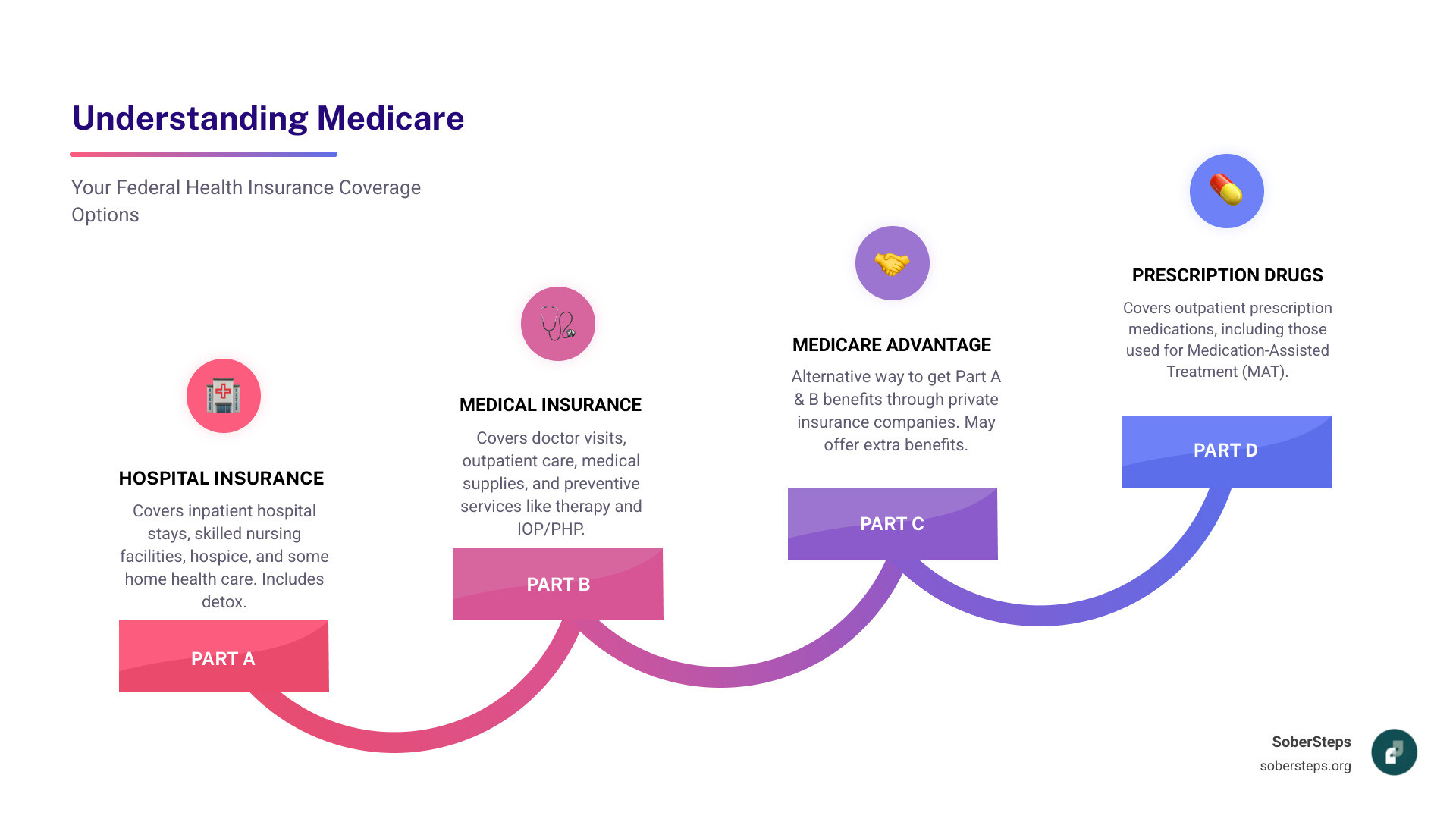
Does Medicare Cover Drug and Alcohol Rehab? The Short Answer is Yes
Yes, Medicare Coverage for Alcohol & Drug Rehab is available, providing a crucial lifeline for many. Medicare is a federal health insurance program for individuals who are 65 or older, younger than 65 with certain disabilities, or any age with End-Stage Renal Disease (ESRD) or ALS.
While Medicare does cover drug and alcohol rehab, it comes with one key condition: the treatment must be deemed “medically necessary” by a doctor. This means a healthcare provider must certify your need for treatment and establish a plan of care.
The Mental Health Parity and Addiction Equity Act (MHPAEA) has also influenced Medicare to expand its mental health and substance use disorder benefits, ensuring that addiction is treated like any other medical condition.
Navigating these requirements can be challenging, but you don’t have to do it alone. At Sober Steps, we can help you understand your benefits and find a Medicare-approved treatment provider. Get Help Now to start your recovery journey.
Breaking Down Medicare Coverage for Alcohol & Drug Rehab by Part
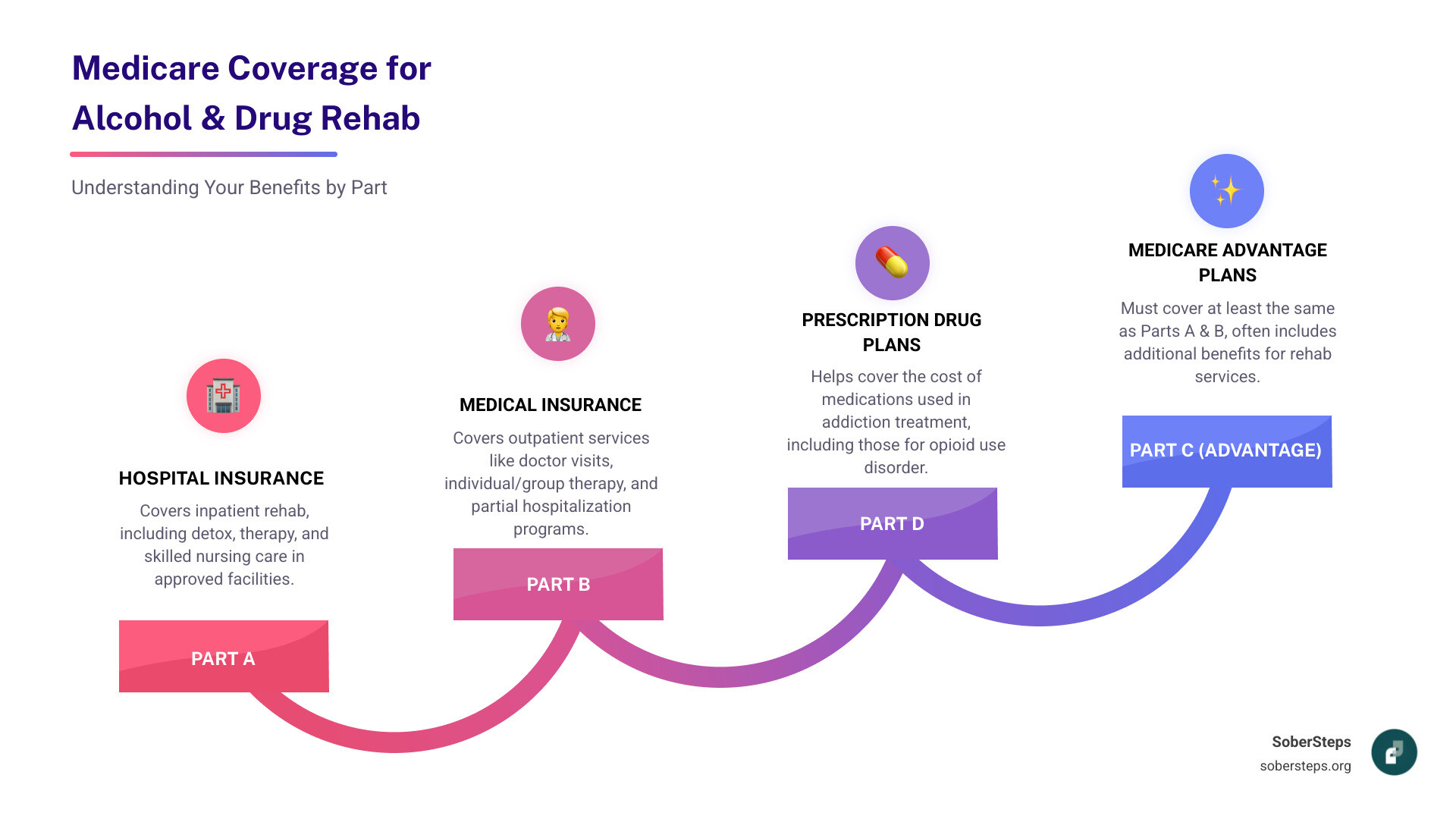
Understanding Medicare Coverage for Alcohol & Drug Rehab means knowing its different “Parts.” We’ll break down Original Medicare (Parts A and B), Medicare Advantage (Part C), and prescription drug coverage (Part D). Each part covers different services, from inpatient stays to outpatient therapy and medication. Knowing which part covers which service is key to accessing the right level of care for your needs. For a complete overview of treatment options, see our guide to Addiction Treatment.
Medicare Part A (Hospital Insurance) for Inpatient Rehab
Medicare Part A (Hospital Insurance) covers inpatient services for addiction treatment. This includes your stay, meals, and nursing care in a hospital or specialized facility. Key services covered are:
- Inpatient Rehab: Stays in a general or psychiatric hospital.
- Medical Detoxification: Medically supervised withdrawal management. Learn more about Detox.
- Associated Costs: Semi-private rooms, meals, nursing care, and medications administered during your stay.
Part A coverage works in “benefit periods.” You’ll pay a deductible for each period (e.g., $1,676 in 2025). After that, days 1-60 are covered. Coinsurance applies for longer stays. Be aware of the 190-day lifetime limit for care in a psychiatric hospital, though this doesn’t apply to mental health care in a general hospital. For official details, visit Medicare.gov.
Medicare Part B (Medical Insurance) for Outpatient Treatment
Medicare Part B (Medical Insurance) covers a wide range of outpatient services for addiction treatment. After you meet your annual Part B deductible, you typically pay 20% of the Medicare-approved amount for most services.
Covered services include:
- Counseling & Therapy: Individual and group therapy with various licensed professionals.
- Doctor’s Visits: Consultations with psychiatrists and other physicians.
- Intensive Outpatient Programs (IOP) & Partial Hospitalization Programs (PHP): Structured treatment programs that allow you to live at home.
- Screenings: Annual alcohol misuse screenings and follow-up counseling.
- SBIRT: Screening, Brief Intervention, and Referral to Treatment services.
As of 2024, more types of mental health professionals, including addiction counselors and marriage and family therapists, can bill Medicare. This makes it easier to Find Addiction Treatment that fits your needs. For more on flexible care, see our Outpatient Treatment guide.
Medicare Part C (Medicare Advantage) & Your Options
Medicare Part C, or Medicare Advantage, are plans from private insurers that bundle Part A, Part B, and often Part D coverage. They must cover everything Original Medicare does but may offer extra benefits like dental or vision.
These plans often use networks like HMOs or PPOs, which can affect your choice of providers and costs. While they must cover medically necessary addiction treatment, their specific rules, copayments, and deductibles vary. Always verify your plan’s specific details before starting treatment. For more on financing your care, read our guide on How Do I Pay for Addiction Treatment?.
Medicare Part D for Addiction Treatment Medications
Medicare Part D provides prescription drug coverage, which is essential for Medicare Coverage for Alcohol & Drug Rehab. These private plans help pay for medications used in Medication-Assisted Treatment (MAT), such as:
- Buprenorphine (e.g., Suboxone) for opioid use disorder (OUD).
- Naltrexone (e.g., Vivitrol) for OUD and alcohol use disorder (AUD).
Part D plans also cover most medications for co-occurring mental health conditions. However, methadone for OUD is a special case; it’s covered under Part B when administered at a certified Opioid Treatment Program (OTP), not through a Part D pharmacy benefit.
Each Part D plan has a list of covered drugs called a formulary. Always check your plan’s formulary to see if your specific medications are included. If you have limited income, you may qualify for the Extra Help program to lower your prescription costs. For more information on OUD, visit our Opioid Addiction page.
What Specific Addiction Treatment Services Does Medicare Cover?

Medicare covers a wide range of medically necessary services to support recovery, from inpatient programs to outpatient therapy. These services are provided in certified Treatment & Rehab Centers and are designed to create a full continuum of care that adapts to your needs. Understanding the difference between inpatient and outpatient coverage is key.
Inpatient vs. Outpatient Programs
Medicare distinguishes between inpatient and outpatient settings, and your coverage will vary accordingly. Here’s a quick comparison:
| Feature | Inpatient Rehab (Part A) | Outpatient Rehab (Part B) |
|---|---|---|
| Setting | Hospital or specialized residential facility. | Clinic, therapist’s office, or hospital outpatient department. |
| Intensity | 24/7 medical and therapeutic supervision. | Scheduled appointments, typically a few hours per day or week. |
| Services | Medically-managed detox, therapy, room and board. | Individual/group therapy, counseling, medication management. |
| Best For | Severe addiction, co-occurring medical issues, or unstable living environment. | Mild to moderate addiction, strong support system at home. |
| Cost | Part A deductible per benefit period, then daily coinsurance after 60 days. | Part B deductible, then 20% coinsurance for most services. |
Specialized Services: OTPs, MAT, and Mental Health
Beyond general rehab, Medicare covers several specialized services:
- Opioid Treatment Programs (OTPs): These SAMHSA-certified clinics provide comprehensive OUD treatment, including medication (like methadone), counseling, and therapy, covered under Medicare Part B. Find a local option on our Methadone Clinic Near Me page.
- Medication-Assisted Treatment (MAT): MAT combines medication with therapy. Buprenorphine and naltrexone are typically covered by Part D, while methadone for OUD is covered under Part B through an OTP.
- Co-occurring Mental Health Disorders: Medicare covers treatment for Dual Diagnosis, where addiction and a mental health condition like depression or anxiety exist together. This includes psychotherapy, Group Therapy, and medication management.
- Telehealth Services: You can receive counseling and other mental health services remotely. Medicare has expanded its coverage for telehealth, making it easier to get help from home. Learn more at Medicare.gov.
Navigating these options can be complex. Sober Steps can connect you with providers who offer the specific treatment you need, from Individual Therapy for Addiction to comprehensive OTP services.
Understanding Costs, Limitations, and How to Get Help
Understanding the costs and limitations of Medicare Coverage for Alcohol & Drug Rehab is key to accessing care. Your out-of-pocket expenses will depend on your specific plan, the provider’s network status, and the type of treatment you receive. For help finding the right program, see our guide on Locating the Best Alcohol Treatment Centers.
Medicare vs. Medicaid for Addiction Treatment
Medicare and Medicaid are often confused, but they are different programs.
- Medicare is a federal program primarily for those 65+ or with certain disabilities, regardless of income. Its rules are generally the same nationwide.
- Medicaid is a joint federal and state program for low-income individuals and families. Eligibility and coverage vary by state.
While both cover addiction treatment, the specifics differ. For more details, see our page on Medicaid Coverage for Rehab or this external resource on their differences.
Dual Eligibility: What if You Have Both Medicare and Medicaid?
If you qualify for both Medicare and Medicaid, you are “dual eligible.” This can significantly reduce your out-of-pocket costs for addiction treatment.
- Medicare pays first as the primary insurer.
- Medicaid acts as the secondary payer, often covering deductibles, copayments, and coinsurance that Medicare doesn’t.
- Medicaid may also cover additional services not included in your Medicare plan.
Being dual eligible can make treatment much more affordable. Contact your State Medicaid office to understand your full range of benefits.
How to Verify Your Specific Medicare Coverage for Alcohol & Drug Rehab
To confirm your specific Medicare Coverage for Alcohol & Drug Rehab, take these steps:
- Call 1-800-MEDICARE: Have your card ready and ask about your benefits for substance use disorder treatment.
- Review Your Plan Documents: For Medicare Advantage (Part C) or Part D plans, check your “Evidence of Coverage” for details on costs and limitations.
- Contact Treatment Centers: An admissions navigator can verify your benefits and estimate your out-of-pocket costs.
- Let Us Help: Verifying insurance can be overwhelming. Our team at Sober Steps can do it for you. Use our free and confidential insurance verification service to understand your coverage and find a compatible treatment center.
Frequently Asked Questions about Medicare and Rehab
We know you likely have more questions, and that’s perfectly normal! Here are some of the most common questions we hear regarding Medicare Coverage for Alcohol & Drug Rehab.
How long will Medicare pay for rehab?
Medicare does not set a specific time limit for rehab. Coverage is based on medical necessity, as determined by your doctor. For inpatient care (Part A), there is a 190-day lifetime limit for care in a psychiatric hospital, but not for treatment in a general hospital. For outpatient services (Part B), there are no time limits as long as the care is medically necessary.
Does Medicare cover treatment for co-occurring mental health disorders?
Yes. Medicare covers treatment for co-occurring mental health disorders, also known as a Dual Diagnosis. This includes services like psychotherapy, counseling, and medication management to treat conditions like depression or anxiety alongside addiction. An integrated approach is essential for lasting recovery. For more information, see our Mental Health Insurance Complete Guide.
What should I do if Medicare denies coverage for my treatment?
If Medicare denies coverage, don’t give up. You have the right to appeal.
- Review the denial letter to understand the reason.
- Work with your healthcare provider to gather supporting medical documents.
- File an appeal by following the instructions in the denial letter. The first step is usually a “Redetermination” request.
Many treatment centers can help you with this process. For more support, visit our Get Help Addiction page.
Conclusion: Taking the Next Step Toward Recovery
Navigating Medicare Coverage for Alcohol & Drug Rehab can feel complex, but Medicare is a powerful resource for your recovery. It offers comprehensive benefits across its different parts, from inpatient detox (Part A) and outpatient therapy (Part B) to prescription medications (Part D).
Key takeaways:
- Yes, Medicare covers addiction treatment when it’s medically necessary.
- Your specific plan (Original Medicare vs. Medicare Advantage) determines your costs and provider network.
- Always verify your coverage with your plan and treatment provider.
- You have the right to appeal any denial of coverage.
Recovery is possible, and insurance should not be a barrier. At Sober Steps, we simplify the process by helping you understand your benefits and connecting you with the right treatment. Your journey to a healthier, sober future can start today. For more on financing your care, review our guide on How Do I Pay for Addiction Treatment?.



