Navigating the Overlap of Mental Health and Substance Use
When mental health problems and substance use happen together, you’ll often hear the terms dual diagnosis vs co-occurring disorders. Here’s what you need to know right away:
Quick Answer:
- Dual Diagnosis = Any two health conditions happening at the same time (can include mental health, substance use, or physical health issues)
- Co-Occurring Disorders = Specifically a mental health disorder AND a substance use disorder happening together
- In Practice = Healthcare providers often use these terms interchangeably, especially in addiction treatment settings
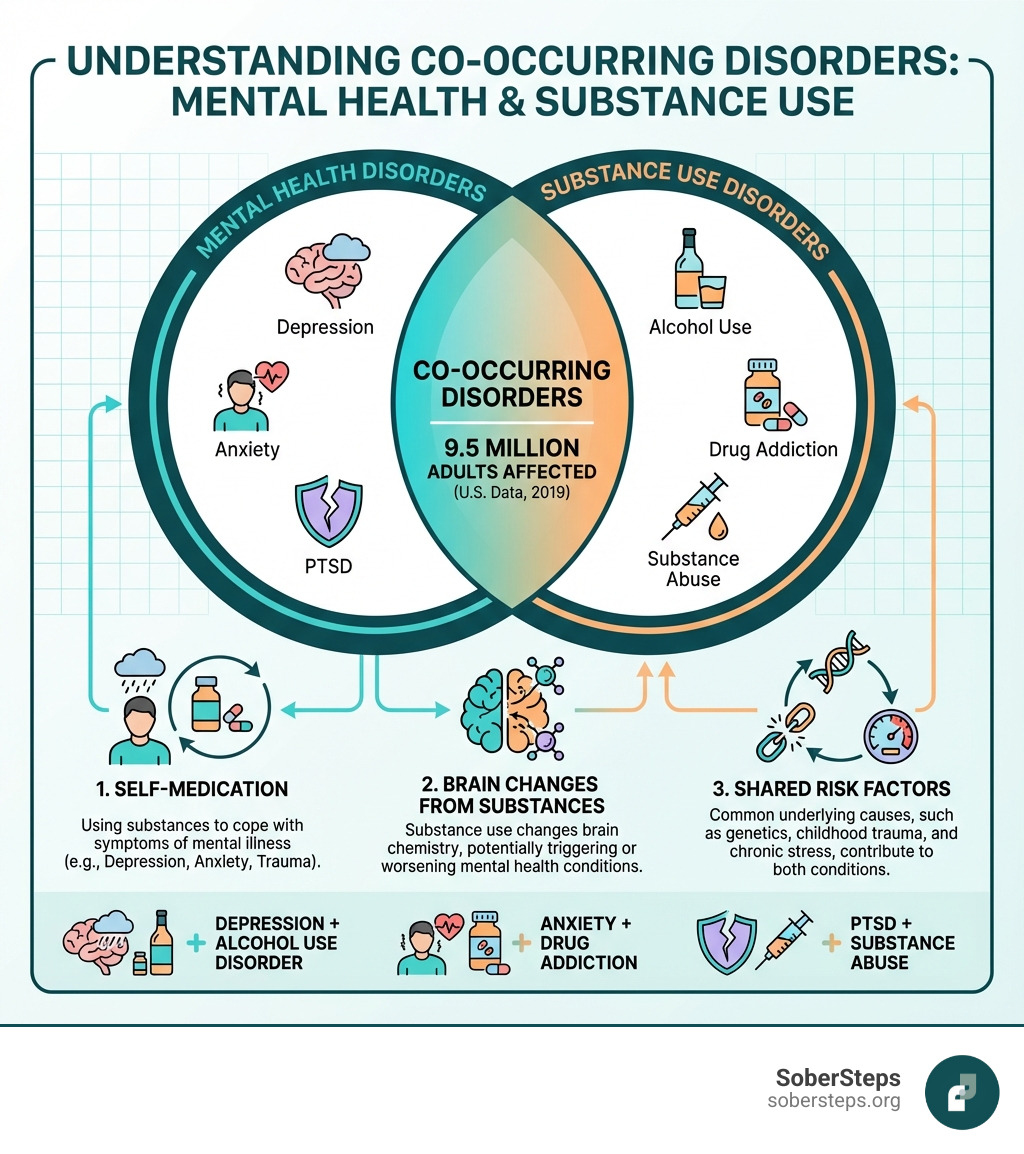
These conditions are incredibly common. In 2019, about 9.5 million U.S. adults experienced both a mental illness and a substance use disorder, which is roughly 1 in 20 adults.
This overlap happens for several reasons. Some people use drugs or alcohol to self-medicate symptoms of depression, anxiety, or trauma. In other cases, substance use can alter brain chemistry, triggering mental health issues. Often, shared risk factors like genetics, trauma, or chronic stress contribute to both conditions.
Getting the terminology right matters. When providers recognize co-occurring disorders, they can create an integrated treatment plan that addresses both issues simultaneously, which is far more effective than treating them separately.
The challenge? Many people receive treatment for only one disorder, or no treatment at all. In 2019, less than half of adults with co-occurring disorders got the help they needed. This gap in care often leads to a frustrating cycle of relapse, as the untreated condition undermines recovery.
At SoberSteps, we’ve spent years helping individuals and families steer the complexities of dual diagnosis vs co-occurring disorders through our comprehensive resources and support network. Our mission is to connect you with accurate information and quality treatment options that address all aspects of your recovery journey.
If you or a loved one are struggling, understanding these terms is your first step toward getting the right kind of help.
Call to Action: If you or a loved one are struggling, reach out to SoberSteps for confidential support. Learn more about our approach to co-occurring disorders.
The Key Difference: Dual Diagnosis vs Co-Occurring Disorders
When discussing mental health and substance use, the terms “dual diagnosis” and “co-occurring disorders” are often used interchangeably. While common in clinical settings, there are subtle yet important distinctions between them that are crucial for a clear understanding.
At its core, both terms refer to the presence of two or more health issues in one person. However, the scope and implication for treatment can vary. Understanding this can help us better steer the path to healing.
| Feature | Dual Diagnosis | Co-Occurring Disorders – |
|---|---|---|
| Definition | A general term for any two or more health conditions diagnosed at the same time. | Specifically refers to having both a mental health disorder and a substance use disorder (SUD) at the same time. – |
| Scope | Broad. Can include any combination of mental, physical, or substance use disorders (e.g., diabetes and depression). | Narrow. Refers only to the combination of a mental health disorder and an SUD. – |
| Relationship | The conditions may be unrelated. The term simply means they exist at the same time. | Implies an interconnected relationship where the conditions influence or worsen each other. – |
| Common Usage | Used in general medicine for any two conditions. Often used interchangeably with “co-occurring disorders” in addiction treatment. | The preferred term by experts like SAMHSA for the specific combination of mental health and substance use disorders. – |
| Treatment Implication | Treatment addresses both conditions, but may not be integrated if they are seen as independent. | Integrated treatment is essential. Treating both conditions together is key to preventing relapse and achieving lasting recovery. – |
Learn more about Co-occurring Disorders Treatment.
Call to Action: Contact SoberSteps for a confidential assessment and to discuss your unique needs.
What is a Dual Diagnosis?
In its broadest sense, a dual diagnosis means having two or more health conditions simultaneously. These can be unrelated, like depression and heart disease. However, in behavioral health, “dual diagnosis” commonly refers to having both a mental health disorder and a substance use disorder (SUD), such as ADHD and an alcohol use disorder. The key is the presence of two distinct diagnoses in one person.
More info about Dual Diagnosis.
What are Co-Occurring Disorders?
Co-occurring disorders specifically refers to having both a mental health disorder and a substance use disorder (SUD) at the same time. The key difference is the implied relationship between the two; one condition often influences or worsens the other. For example, someone with anxiety might use alcohol to self-medicate, or substance abuse might trigger depression. This interconnectedness is why organizations like the Substance Abuse and Mental Health Services Administration (SAMHSA) prefer this term, as it highlights the need for integrated treatment. According to SAMHSA, this is a common issue, highlighting the need for integrated treatment approaches.
Common co-occurring disorders include:
- Anxiety disorders and alcohol dependence
- Depression and opioid addiction
- Bipolar Disorder and stimulant use disorder
- Post-Traumatic Stress Disorder (PTSD) and cannabis abuse
- Schizophrenia and polysubstance abuse
- Borderline Personality Disorder and various SUDs
Call to Action: Explore our Dual Diagnosis resources for more information.
Why the Distinction in Dual Diagnosis vs Co-Occurring Disorders Matters for Treatment
This distinction matters for treatment. Recognizing conditions as “co-occurring” highlights a deep, often causal, relationship that requires integrated care. Historically, mental health and addiction were treated separately, leading to fragmented care and poor outcomes. Treating one condition while ignoring the other is like trying to fix a leak while the water is still running.
The untreated disorder often triggers a relapse in the other. For example, unmanaged depression can lead back to substance use as a coping mechanism. An accurate diagnosis and an integrated approach are crucial to address both conditions simultaneously, preventing this cycle and enabling sustainable recovery. This is why integrated Behavioral Health Support is the foundation of successful treatment.
Call to Action: Connect with SoberSteps to get matched with the right support for your situation.
Common Conditions and Underlying Causes
The intricate link between mental health and substance use disorders isn’t random. It’s a complex interplay of biology, psychology, and environment.
The “self-medication hypothesis” suggests people use substances to cope with mental health symptoms. For example, using alcohol to ease anxiety or opioids to numb depression. This provides temporary relief but ultimately worsens both conditions and can lead to a substance use disorder (SUD).
Beyond self-medication, shared risk factors also play a major role. Genetics, a difficult social environment, trauma, or chronic stress can increase the risk for both mental health disorders and SUDs, creating fertile ground for them to co-occur.
Common Mental Health Disorders That Co-Occur with SUDs
Some mental health disorders are frequently seen alongside substance use due to their significant impact and high prevalence.
- Depression: Can be both a cause and a consequence of substance use, as individuals may use substances to cope with feelings of sadness and hopelessness.
- Anxiety Disorders: Individuals often use alcohol or drugs to manage symptoms of panic, worry, or social fear, creating a cycle where substance use worsens anxiety over time.
- Bipolar Disorder: The intense mood swings of bipolar disorder can lead to substance use to either self-medicate depressive lows or manage manic episodes. Impulsivity during mania also increases risk.
- Post-Traumatic Stress Disorder (PTSD): Trauma is a major risk factor. People with PTSD may use substances to numb painful memories, flashbacks, and anxiety. Research shows a strong link between PTSD and SUDs.
- Schizophrenia: Individuals with schizophrenia have a high rate of co-occurring SUDs, sometimes using substances to manage symptoms like hallucinations or medication side effects.
- Borderline Personality Disorder: The emotional instability and impulsivity of BPD often lead to substance use as a way to cope with intense feelings or a sense of emptiness.
Call to Action: Find out how SoberSteps addresses these conditions.
How Genetics and Environment Contribute
The development of dual diagnosis vs co-occurring disorders is rarely due to a single factor. It’s a complex interplay of genetic predispositions and environmental influences.
Genetics play a significant role. Research indicates that about 50% of the risk for addiction is hereditary. Similarly, many mental health conditions have a genetic component, as highlighted by research from the National Institute of Mental Health. A family history of either condition increases an individual’s risk.
Environmental factors are just as crucial. Trauma and chronic stress, particularly in childhood, are strong predictors for both SUDs and mental illness. For instance, over 60% of adolescents in substance use treatment also have another mental health diagnosis. The adolescent brain is especially vulnerable. Early substance use can alter brain development, increasing the risk for both addiction and mental health issues later in life. Substance use can also cause epigenetic changes, which affect how genes are expressed and can influence a person’s response to drugs and their risk of developing tolerance.
Call to Action: Explore our resources to learn more about the science behind dual diagnosis and co-occurring disorders.
Finding the Right Path: Treatment for Co-Occurring Conditions
The good news is that recovery from dual diagnosis vs co-occurring disorders is possible with a specialized, integrated approach. Treating mental health and substance use disorders separately is often ineffective, as one condition can trigger a relapse in the other. Integrated treatment addresses both conditions simultaneously, with the same team, in the same setting. This cohesive approach acknowledges their complex interplay. Accurate diagnosis is vital, and studies show that integrated care significantly improves long-term outcomes and quality of life.
Learn about our treatment options.
Integrated Treatment Approaches
Integrated care is the gold standard for treating co-occurring disorders. It combines mental health and substance use interventions into one comprehensive treatment plan. This avoids the pitfalls of separate (sequential or parallel) treatment, which can lead to gaps in care and poorer outcomes.
The benefits of integrated care are numerous:
- Holistic Healing: It addresses the individual as a whole, recognizing that mental health and substance use are interconnected.
- Reduced Relapse Risk: By treating both conditions concurrently, the risk of one disorder triggering a relapse in the other is significantly reduced.
- Improved Outcomes: Patients in integrated programs often show greater reductions in psychiatric symptoms and substance use, along with improved overall functioning.
- Coordinated Care: A unified treatment team ensures consistent messaging, avoids conflicting advice, and provides seamless support.
While implementing integrated care can be resource-intensive, the long-term benefits for patient well-being are undeniable. Finding a Mental Health Clinic that offers these specialized services is a crucial first step.
Call to Action: Start your recovery journey with SoberSteps—our team can help you find integrated care custom to your needs.
Effective Therapies and Interventions
A variety of evidence-based therapies are highly effective in treating dual diagnosis vs co-occurring disorders as part of an integrated plan:
- Cognitive Behavioral Therapy (CBT): Helps patients identify and change negative thought patterns and behaviors linked to both substance use and mental health issues.
- Dialectical Behavior Therapy (DBT): Especially effective for those with intense emotions and self-harming behaviors, DBT teaches skills in mindfulness, emotional regulation, and distress tolerance.
- Motivational Interviewing (MI): A client-centered approach that helps individuals find their own motivation to change and commit to treatment for both disorders.
- Role of Medication: Medications can be vital for managing mental health symptoms (e.g., antidepressants, mood stabilizers) and aiding in substance use recovery (e.g., medications for cravings). Some medications can even treat both conditions simultaneously.
- Support Groups: Peer support from groups like Alcoholics Anonymous (AA), Narcotics Anonymous (NA), and Dual Recovery Anonymous (DRA) provides a community of shared experience. DRA is specifically for individuals with co-occurring disorders.
- Individual Therapy: One-on-one sessions offer a private setting to address personal issues, develop coping skills, and work through trauma.
Call to Action: Discover which therapies may be right for you.
Levels of Care: Inpatient, Outpatient, and More
Choosing the right level of care is crucial for treating dual diagnosis vs co-occurring disorders. The best setting depends on symptom severity, support systems, and personal needs. Treatment often follows a continuum, stepping down from more intensive care as the individual stabilizes.
- Detoxification: The first step for many, providing safe, medically supervised management of withdrawal symptoms to prepare for further treatment.
- Inpatient Rehab: Provides 24/7 support in a residential setting for those with severe symptoms, allowing for an intensive focus on recovery.
- Partial Hospitalization Programs (PHP): A step down from inpatient care, offering structured day treatment while allowing patients to live at home.
- Intensive Outpatient Programs (IOP): A flexible option with fewer hours than PHP, allowing individuals to maintain work or school commitments while in treatment.
- Sober Living: Supportive, substance-free housing that helps bridge the gap between intensive treatment and independent living.
- Aftercare and Relapse Prevention: Long-term support for a lifelong journey. Includes ongoing therapy, support groups, and relapse prevention strategies.
Call to Action: Find the right level of care for you—SoberSteps can guide you every step of the way.
Practical Advice for Individuals and Families
Dealing with dual diagnosis vs co-occurring disorders is challenging for both the individual and their loved ones. The journey can be emotionally and financially draining, but with the right approach, family and friends can become powerful allies in recovery.
How to Support a Loved One
Supporting someone with co-occurring disorders requires patience, understanding, and a strategic approach. Here’s how you can help:
- Educate Yourself: Learn about your loved one’s specific conditions. Understanding the symptoms and triggers will help you respond with more empathy and effectiveness.
- Encourage Professional Help: Gently encourage your loved one to seek integrated treatment for both conditions. Resources like SAMHSA’s National Helpline (1-800-662-HELP) can provide guidance.
- Offer Practical Support: Help with research, provide transportation, or attend appointments with them. This can remove significant barriers to getting care.
- Foster a Supportive Environment: Make your home a safe space for recovery by removing substances and encouraging healthy habits. Supporting their treatment efforts is key. Tips for helping a loved one stay sober can provide more ideas.
- Practice Self-Care: Supporting someone is demanding. It’s crucial to care for your own well-being by setting boundaries and seeking support for yourself. Finding Confidential Mental Health Support is a necessary step for caregivers.
Call to Action: Support your loved one with SoberSteps resources.
Choosing the Right Treatment Path for Dual Diagnosis vs Co-Occurring Disorders
Selecting the appropriate treatment path is a critical, personal decision. Here are key factors to consider:
- Assess Symptom Severity: The intensity of symptoms determines the necessary level of care. Severe symptoms may require inpatient or detox services, while milder cases might be suited for outpatient care.
- Consider Personal Preferences: Engagement is key to success. Discuss preferences for therapy styles, program structure, and location to find the best fit.
- Evaluate Support Systems: A strong support network of family and friends is a major asset in recovery. Look for programs that involve these supports.
- Verify Your Mental Health Insurance: Understand your insurance coverage for integrated treatment to avoid unexpected costs. Verify your benefits before starting a program.
- Seek Specialized Programs: Look for facilities that offer integrated treatment for dual diagnosis vs co-occurring disorders. This ensures the staff and program are equipped to handle both conditions. Finding Addiction Treatment that specializes in this is crucial.
The goal is a comprehensive, person-centered plan that evolves with the individual’s needs throughout their recovery journey.
Call to Action: Connect with SoberSteps for a confidential assessment and personalized treatment recommendations.
Frequently Asked Questions about Dual Diagnosis and Co-Occurring Disorders
What is the main difference between dual diagnosis and co-occurring disorders?
While often used interchangeably, “dual diagnosis” is a broad term for any two simultaneous health conditions. “Co-occurring disorders” is more specific, referring to the presence of both a mental health disorder and a substance use disorder. The term implies a clinical relationship where the conditions influence each other.
Why is it better to treat both conditions at the same time?
Integrated treatment is crucial because mental health and substance use disorders often fuel each other. Treating only one can lead to relapse, as the untreated condition remains a trigger. For example, untreated anxiety can lead back to substance use. An integrated approach breaks this cycle, leading to better long-term recovery outcomes and improved quality of life.
Can you recover from a co-occurring disorder?
Yes, long-term recovery is absolutely achievable. With a comprehensive, integrated treatment plan—including therapy, medication, and support groups—individuals can learn to manage both conditions effectively. Recovery is an ongoing journey, and with consistent support, a fulfilling life is possible.
Call to Action: Have more questions? Contact SoberSteps now for answers and support.
Take the First Step Towards Integrated Healing
Understanding the nuances of dual diagnosis vs co-occurring disorders is the first step. The key takeaway is that when mental health and substance use issues exist together, they must be treated together.
Integrated treatment is not just a preference—it’s the most effective path to breaking the cycle of relapse and building a foundation for lasting recovery. We’ve seen how addressing both conditions simultaneously empowers individuals to find sustainable healing.
There is immense hope for recovery, and your journey to wellness can start today. Taking that first step can be daunting, but you don’t have to do it alone. SoberSteps is here to guide you, offering a confidential helpline to connect you with experienced treatment providers who specialize in integrated care for co-occurring disorders.
Call to Action: Don’t wait—take the first step with SoberSteps and start building your path to recovery today. For more information, visit our Dual Diagnosis and Co-occurring Disorders Treatment pages. Explore our comprehensive Co-occurring Disorders Treatment guide.




