
Why a Specialized Plan is Crucial for Recovery
A dual diagnosis treatment plan is a comprehensive approach for individuals with both a mental health disorder and a substance use disorder (SUD). This condition is also called co-occurring disorders.
The connection is common: approximately 50 percent of people with serious mental disorders are also affected by substance abuse. Many people with mental illness turn to substances to self-medicate painful emotions or thoughts, but this often worsens symptoms over time, creating a vicious cycle. Likewise, chronic substance use can alter brain chemistry, triggering or worsening mental health conditions.
Treating these conditions separately doesn’t work. Fragmented care leads to higher rates of relapse, hospitalization, and other negative outcomes. The solution is integrated treatment, where one team addresses both conditions simultaneously. This approach is proven to reduce substance use, improve psychiatric symptoms, and increase overall quality of life.
Key Components of an Effective Plan:
- Integrated Assessment – A full evaluation of both mental health and substance use.
- Medically Supervised Detox – Safe withdrawal management with psychiatric monitoring.
- Stabilization – Structured residential or intensive outpatient care.
- Behavioral Therapies – CBT, DBT, and trauma-informed counseling for both conditions.
- Medication Management – Coordinated pharmacotherapy for mental health and addiction.
- Support Systems – Peer groups, family therapy, and community resources.
- Aftercare Planning – Long-term relapse prevention and mental health support.
At Sober Steps, we are dedicated to helping you steer recovery from co-occurring disorders. Our platform connects you with evidence-based information and treatment options that address both conditions at once.
Explore dual diagnosis treatment options now or get immediate help through our 24/7 helpline.
Understanding Dual Diagnosis: The Foundation of Your Treatment
A dual diagnosis, or co-occurring disorders, means having both a mental health condition and a substance use disorder at the same time. These conditions are often deeply intertwined, and understanding this connection is the first step toward an effective dual diagnosis treatment plan.

These disorders often occur together for several reasons. Common risk factors like genetics, stress, and trauma can predispose individuals to both. Mental health disorders can also lead to substance use as a form of “self-medication” to cope with symptoms, which can then lead to addiction. Conversely, chronic substance use can alter brain chemistry, triggering or worsening mental illnesses. This complex, bidirectional relationship is why an integrated approach is vital.
For more details, explore scientific research on co-occurring disorders and dig into more info about Dual Diagnosis.
Differentiating Addiction Treatment from Dual Diagnosis Programs
It’s crucial to choose the right program. Here’s how standard addiction treatment differs from a specialized dual diagnosis program:
| Feature | Standard Addiction Treatment Program | Dual Diagnosis Program |
|---|---|---|
| Primary Focus | Stopping substance use and maintaining sobriety. | Simultaneously addressing both substance use and co-occurring mental health disorders. |
| Therapeutic Approach | Often relies on 12-step philosophies and counseling focused on addiction and relapse prevention. | Integrates addiction therapies with evidence-based mental health treatments (CBT, DBT, trauma therapy) within a psychiatric framework. |
| Staff Expertise | Addiction counselors and staff specializing in substance use recovery. | Multidisciplinary team including psychiatrists, psychologists, and therapists trained in both mental health and substance use disorders. |
| Assessment Process | Focuses on substance use history. May screen for mental health issues but often refers out for in-depth evaluation. | Comprehensive psychiatric and substance use assessment to diagnose both conditions and understand their interaction. |
| Ideal Candidate | Individuals whose primary challenge is substance dependence with minimal co-occurring mental health symptoms. | Individuals with significant mental health symptoms that contribute to, or are worsened by, substance use. |
While a standard program is great for focusing on substance use, a dual diagnosis program addresses the underlying mental health issues that are often intertwined. If you’re unsure which is right for you, we can help you find the right type of rehab for you.
Do You Need a Dual Diagnosis Program?
Consider if a dual diagnosis treatment plan is what you need:
- Worsening Mental Health in Sobriety: If stopping substance use makes your anxiety or depression unbearable, it’s a strong sign you need integrated treatment.
- Using Substances to Cope: Do you use alcohol or drugs to manage sadness, panic, or trauma? This “self-medication” is a classic sign of co-occurring disorders.
- History of Trauma: Unresolved trauma often leads to substance use as a coping mechanism. Treating both simultaneously is most effective.
- Previous Failed Treatment Attempts: If you’ve relapsed after addiction treatment, an untreated mental health condition may have been a factor.
- Recreational Use and Mental Illness: Even recreational use of substances can impact brain chemistry, interact with medications, and destabilize your mood if you have a mental illness.
The best way to know for sure is through a professional psychiatric assessment. A mental health professional can clarify the relationship between your substance use and psychiatric symptoms to tailor the most effective plan.
If this resonates with you, please don’t hesitate to reach out. Get Help Now and let us connect you with the right support.
The Core Components of a Dual Diagnosis Treatment Plan
An effective dual diagnosis treatment plan requires an integrated, multidisciplinary team approach. At SoberSteps, we follow a “no wrong door” policy, ensuring that no matter why you seek help, you’ll be screened for both mental health and substance use and guided to comprehensive care. Your plan will be customized to you, and we offer various levels of care to match your needs.

Step 1: Comprehensive Assessment and Detoxification
Recovery begins with a thorough assessment of your medical history, psychiatric symptoms, and substance use patterns. This evaluation helps us differentiate between substance-induced symptoms and underlying mental health conditions, forming the foundation of your personalized dual diagnosis treatment plan.
If needed, the next step is medically supervised Detox. Detoxing alone can be dangerous, especially from alcohol, opioids, or benzodiazepines. Our medical team provides 24/7 monitoring to manage withdrawal symptoms safely, which allows us to see your true mental health state without the influence of substances.
Step 2: Stabilization and Level of Care
After detox, the focus shifts to stabilization in a safe, structured environment. Depending on your needs, this may involve different levels of care:
- Residential Stabilization (Inpatient Treatment): Inpatient treatment offers 24/7 support, therapy, and medical care, providing structure that is especially helpful during post-acute withdrawal syndrome (PAWS).
- Partial Hospitalization Programs (PHP): A Partial Hospitalization Program provides intensive daily treatment while you live at home.
- Intensive Outpatient Programs (IOP): Intensive Outpatient Programs offer structured therapy several times a week, allowing you to maintain daily responsibilities.
Step 3: Integrated Behavioral Therapies
Therapy is the cornerstone of a dual diagnosis treatment plan. We use evidence-based therapies adapted for co-occurring disorders:
- Cognitive Behavioral Therapy (CBT): Helps you identify and change negative thought patterns and behaviors linked to both mental health and substance use.
- Dialectical Behavior Therapy (DBT): Teaches skills in mindfulness, distress tolerance, and emotion regulation to manage intense emotions and cravings.
- Motivational Interviewing (MI): A client-centered approach that helps you find your own motivation for recovery.
- Trauma-Informed Care: Our therapies are delivered with an understanding of how past trauma impacts present behaviors.
- Individual Therapy: One-on-one sessions to explore personal issues and develop coping skills.
- Group Therapy: Offers peer support and a sense of community with others facing similar challenges.
Step 4: Medication Management
Medication can be a vital part of a dual diagnosis treatment plan. Our psychiatrists integrate pharmacotherapy for both conditions.
- Medications for Substance Use Disorder (SUD): FDA-approved medications are available to reduce cravings and prevent relapse for opioid, alcohol, and nicotine dependence.
- Medications for Mental Health: Antidepressants, mood stabilizers, and other psychiatric medications can effectively manage symptoms of depression, bipolar disorder, or anxiety, making it easier to engage in recovery.
A psychiatrist will carefully assess your needs, prescribe appropriate medications, and monitor for effectiveness and potential interactions. This coordinated approach is key to holistic care. Learn more about Substance Abuse Treatment and the role medication can play.
Step 5: Building a Support System
Recovery isn’t a journey you take alone. A strong support system is crucial.
- Peer Support Groups: Groups like Double Trouble in Recovery (DTR) and Dual Recovery Anonymous (DRA) are designed for individuals with co-occurring disorders. You can also explore Online NA Meetings and other online recovery support groups.
- Family Therapy: Helps improve communication, set healthy boundaries, and educate loved ones about dual diagnosis.
A robust support network provides the encouragement and accountability vital for long-term recovery.
Tailoring the Plan for Specific Co-Occurring Disorders
While the core components of a dual diagnosis treatment plan are consistent, the specific therapies and medications are customized to your primary mental health diagnosis. This personalized approach is key to effective Co-occurring Disorders Treatment.
Interventions for Bipolar Disorder and Substance Use
For co-occurring bipolar disorder, where substances can destabilize mood, our integrated approach focuses on:
- Integrated Group Therapy (IGT): A specialized therapy that combines psychoeducation, relapse prevention, and coping skills to manage both mood swings and cravings.
- Interpersonal and Social Rhythm Therapy (IPSRT): Focuses on stabilizing daily routines (sleep, meals, social interaction) to improve mood stability.
- Medication Management: Careful management of mood stabilizers and other medications is paramount to achieving stability.
For more, see the Mayo Clinic’s expert answers on Bipolar Disorder and Alcoholism or learn more on Dual Diagnosis Bipolar Disorder.
Interventions for Psychotic Disorders and Substance Use
Treating co-occurring psychotic disorders like schizophrenia requires a specialized approach, as substances can worsen symptoms.
- Modified CBT: CBT is adapted to be more precise and repetitive, focusing on practical skills for managing both psychosis and substance use triggers.
- Social Skills Training: Helps reduce the isolation that can trigger substance use.
- Assertive Community Treatment (ACT): An intensive, evidence-based outreach program where a multidisciplinary team provides comprehensive support in the community.
Learn more on Dual Diagnosis Schizophrenia.
Crafting a dual diagnosis treatment plan for Anxiety, Depression, or PTSD
Our dual diagnosis treatment plan for these common co-occurring conditions focuses on addressing underlying emotional pain.
- Targeting Avoidance Behaviors: Therapy helps you safely confront uncomfortable feelings or situations without using substances.
- Exposure Therapy: Particularly effective for anxiety and PTSD, this therapy gradually exposes you to feared situations to reduce their emotional power.
- EMDR (Eye Movement Desensitization and Reprocessing): A highly effective therapy that helps process traumatic memories, reducing the urge to self-medicate.
- Addressing Hopelessness: For depression, therapy focuses on challenging negative thoughts and finding joy in life without substances.
We have dedicated resources for Dual Diagnosis PTSD, Dual Diagnosis Depression, and Dual Diagnosis Anxiety.
Long-Term Recovery: Aftercare and Family Involvement
Completing an intensive program is a major accomplishment, but recovery is a lifelong journey. A robust aftercare plan and family support are essential for long-term success. We understand that recovery is a continuum, and our focus is on sustaining motivation and providing ongoing support.
Learn more about Aftercare planning and how we can support you.
Developing a Continuing Care and Relapse Prevention Plan
Your dual diagnosis treatment plan transitions into a continuing care plan to support you in the real world. This might include:
- Step-Down Levels of Care: Gradually moving from inpatient to outpatient care provides consistent support during reintegration.
- Sober Living Homes: These structured environments foster independence while maintaining accountability in early recovery.
- Ongoing Therapy: Continuing individual or group therapy reinforces coping skills and addresses new challenges.
- Alumni Programs: Stay connected and motivated through a community of support from your treatment center.
- Identifying Triggers and Coping Strategies: A key part of your plan is learning your unique triggers and building a “tool kit” of healthy ways to manage stress and cravings.
Developing strong Relapse Prevention skills is essential for long-term recovery.
The Role of Family in Supporting Recovery
Family involvement can be a powerful force in recovery. Support for loved ones often includes:
- Setting Healthy Boundaries: Defining and maintaining clear limits on acceptable behavior is crucial for everyone.
- Avoiding Enabling: Loved ones learn to stop shielding the individual from consequences while still offering support.
- Participating in Family Therapy: A safe space to improve communication, heal, and learn new ways of interacting.
- Using Support Groups: Groups like Al-Anon or Nar-Anon offer guidance and community for family members.
For more advice, see how to help a loved one stay sober.
Frequently Asked Questions about Dual Diagnosis Treatment
Navigating dual diagnosis brings up many questions. Here, we address common inquiries about dual diagnosis treatment plans.
Should someone with a mental illness abstain from all alcohol and marijuana?
While this is an individual decision to be made with a medical professional, we generally advise caution. Here’s why:
- Medication Impact: Alcohol and marijuana can interfere with psychiatric medications, reducing their effectiveness or causing dangerous side effects.
- Symptom Worsening: These substances can destabilize mood in disorders like bipolar disorder or trigger psychosis in those with schizophrenia. Even without addiction, they can worsen anxiety and depression.
- Individual Risk: The right choice depends on your specific diagnosis, medications, and personal risk factors.
Always consult a medical professional to make an informed decision. For more, read about the link between marijuana and psychiatric disorders.
What are the benefits of integrated treatment?
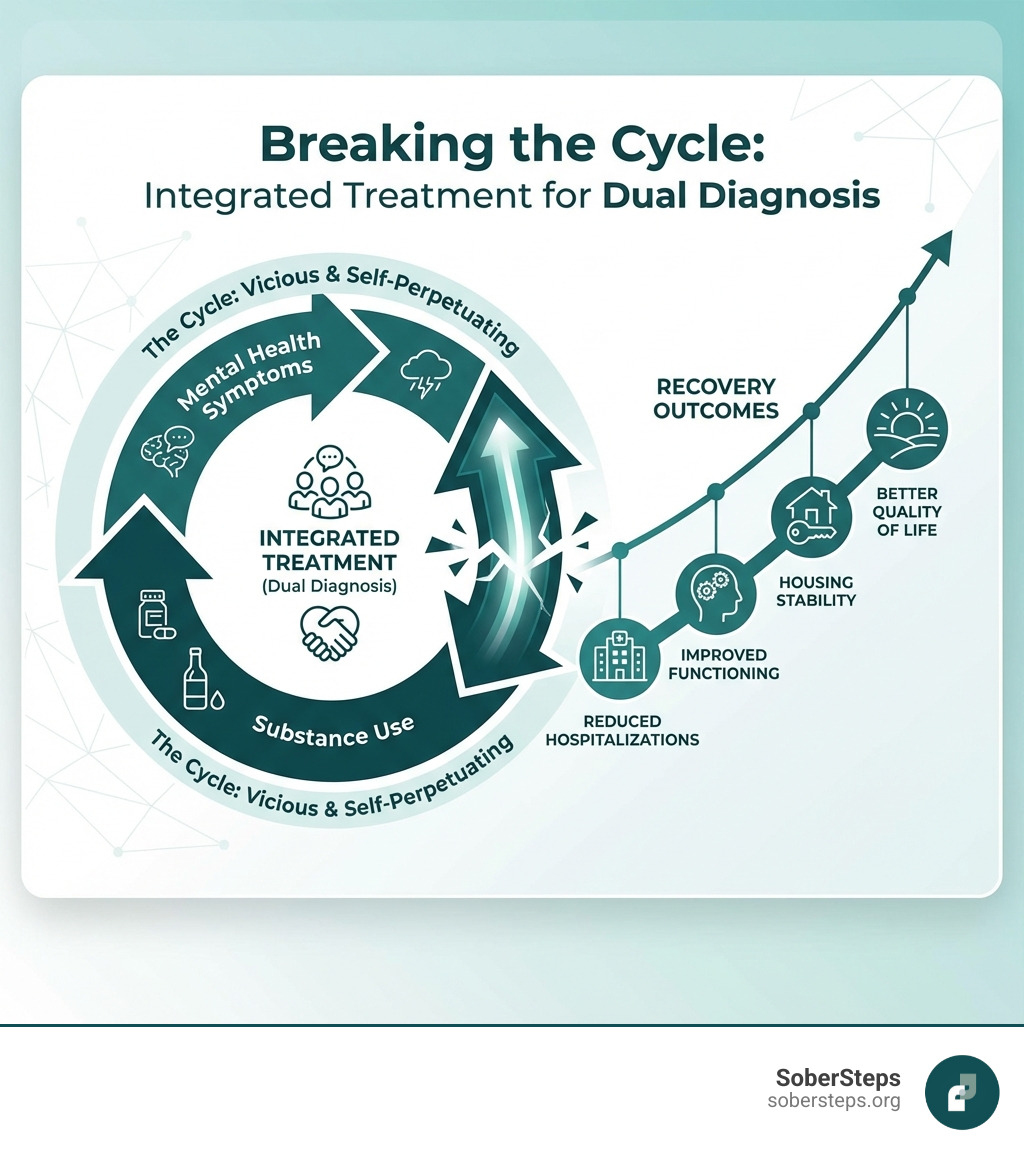
An integrated dual diagnosis treatment plan offers substantial, research-backed benefits, leading to significantly better outcomes:
- Reduced Hospitalizations and Substance Use
- Improved Psychiatric Symptoms and Daily Functioning
- Increased Housing Stability and Quality of Life
- Higher Treatment Retention
- Safer Medication Management
Integrated treatment is the gold standard because it addresses the whole person, leading to more effective and lasting recovery.
How do I pay for a dual diagnosis treatment plan?
Cost is a common concern, but options are available to ensure financial barriers don’t prevent you from getting help.
- Insurance: Many plans cover dual diagnosis treatment. Our Mental Health Insurance Guide can help, and we can assist with Verifying Your Insurance Coverage.
- State-Funded Programs: Many states offer publicly funded treatment based on income or other criteria.
- Other Options: Look into Free Rehab Options or ask treatment centers about payment plans and sliding scale fees.
Don’t let cost deter you. We can help you find resources that fit your financial situation.
Take the First Step Toward Integrated Recovery
Navigating co-occurring disorders is overwhelming, but recovery is within your reach. An integrated dual diagnosis treatment plan offers a clear, evidence-based path to healing. By addressing your mental health and substance use simultaneously, you can break the cycle and build a foundation for a healthier, more fulfilling life.
At SoberSteps, we are an independent platform dedicated to empowering you with knowledge and connecting you to effective treatment and recovery options.
You don’t have to do this alone. Take the courageous first step today. Our confidential 24/7 helpline can connect you with paid advertiser treatment providers who will build a personalized dual diagnosis treatment plan for your unique needs. Recovery begins here.



