
Understanding Dual Diagnosis and Where to Find Help
Dual diagnosis resources connect people struggling with both mental health conditions and substance use disorders to the specialized care they need. These essential tools include federal helplines, treatment locators, therapy programs, and support groups designed specifically for co-occurring disorders.
Quick Access to Key Dual Diagnosis Resources:
- SAMHSA National Helpline: 1-800-662-HELP (4357) – Free, confidential, 24/7 treatment referrals
- 988 Suicide & Crisis Lifeline: Call or text 988 for immediate mental health crisis support
- Treatment Locator: SAMHSA’s FindTreatment.gov helps find nearby programs
- Integrated Treatment Programs: Look for facilities treating both conditions simultaneously
- Support Groups: AA, NA, and SMART Recovery offer peer support for recovery
If you’re dealing with both addiction and mental health challenges, you’re not alone. Research shows that approximately 8 million adults in the United States have a dual diagnosis. This means they’re facing both a mental illness like depression or anxiety and a substance use disorder at the same time.
The good news? Recovery is absolutely possible when both conditions are treated together through integrated care.
Why addressing both conditions matters:
- Mental health symptoms often trigger substance use as a coping mechanism
- Substance use can worsen mental health symptoms
- Treating only one condition typically leads to relapse
- Integrated treatment improves outcomes and quality of life
At Sober Steps, we understand how overwhelming it can be to steer treatment when you’re dealing with co-occurring disorders, which is why we’ve built a comprehensive directory of dual diagnosis resources and treatment facilities to help you find the right support. Our platform connects individuals and families to evidence-based care options and educational materials that make the recovery journey clearer and more manageable.
The Complex Link Between Mental Health and Substance Use
It’s no secret that our minds and bodies are intricately connected, but when it comes to mental health conditions and substance use disorders, this connection becomes even more complex. These conditions often appear together, making diagnosis and treatment a real puzzle. We’re not talking about one causing the other in a simple way, but rather a tangled web of shared vulnerabilities, coping mechanisms, and biological changes that make it difficult to disentangle. Understanding this link is the first step toward finding effective dual diagnosis resources.
Common Co-Occurring Disorders
When we talk about dual diagnosis, we’re referring to any combination of a mental health condition and a substance use disorder (SUD). While any pairing is possible, some are more commonly seen together. For example, individuals struggling with depression may turn to alcohol or drugs to numb their emotional pain, leading to a Depression Dual Diagnosis. Similarly, the constant worry and panic of anxiety can drive someone to self-medicate, resulting in an Anxiety Dual Diagnosis.
Other frequent pairings we encounter include:
- Bipolar Disorder Dual Diagnosis, where individuals may use substances to stabilize mood swings or cope with manic or depressive episodes.
- PTSD Dual Diagnosis often sees individuals using substances to escape traumatic memories or reduce hypervigilance.
- More severe mental illnesses like Schizophrenia Dual Diagnosis can involve substance use to manage hallucinations or delusions.
- Personality disorders such as Borderline Personality Disorder Dual Diagnosis are frequently complicated by substance use as a way to cope with intense emotions and unstable relationships.
- Even neurodevelopmental conditions like ADHD Dual Diagnosis can lead to substance use, sometimes to self-stimulate or self-medicate for focus issues.
If you recognize any of these patterns in yourself or a loved one, it’s a strong indicator that exploring dual diagnosis resources is a crucial next step.
Potential Causes and Contributing Factors
Why do these conditions so often go hand-in-hand? It’s rarely one single cause, but a blend of factors that create a fertile ground for dual diagnosis.
One significant factor is shared risk factors. For instance, both mental illnesses and substance use disorders can have a genetic component. Research suggests a significant genetic heritability of addiction, meaning some individuals are predisposed to developing these issues based on their family history. Environmental factors also play a huge role. Experiencing trauma, chronic stress, or growing up in an unstable environment can significantly increase the risk for both mental health challenges and substance use.
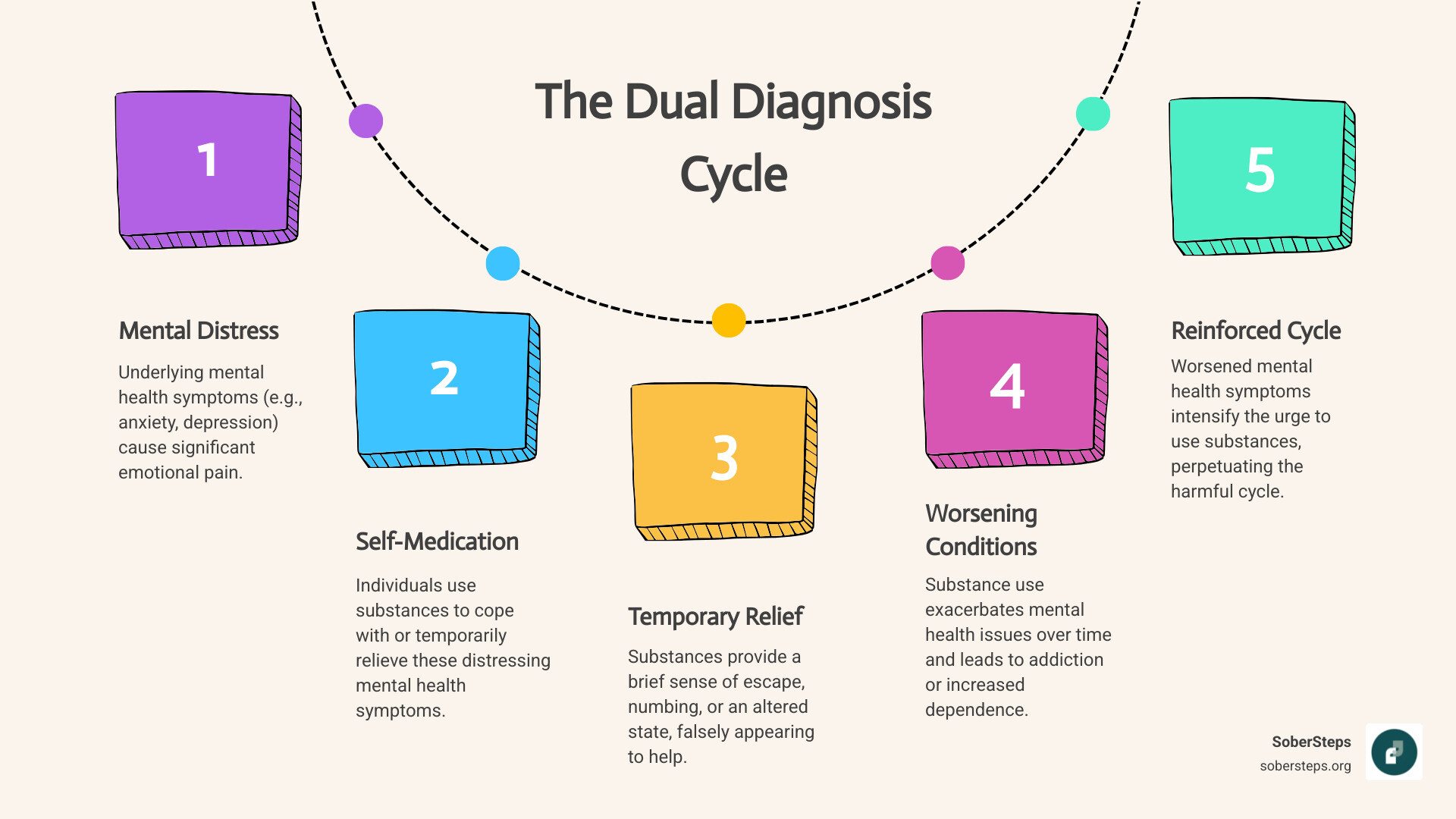
The “self-medication hypothesis” is another key piece of the puzzle. This theory suggests that individuals with mental health symptoms (like anxiety, depression, or even psychosis) may turn to substances to temporarily alleviate their distress. While it might provide short-term relief, this often leads to a vicious cycle where substance use actually worsens the underlying mental health condition over time.
Furthermore, substance use itself can cause changes in the brain that either trigger or exacerbate mental health disorders. As the National Institute of Mental Health explains, how substance use disrupts the brain can alter mood regulation, impulse control, and cognitive function, making individuals more vulnerable to mental illness.
Signs and Symptoms of a Dual Diagnosis
Identifying a dual diagnosis can be tricky because the symptoms often overlap or mimic each other. For example, depression can cause fatigue and lack of motivation, which might also be side effects of substance abuse. This difficulty in diagnosis is why integrated care is so vital.
However, there are common signs and symptoms that might suggest a dual diagnosis:
- Sudden behavioral changes: Unexplained mood swings, increased irritability, or a significant shift in personality.
- Social withdrawal: Pulling away from friends, family, and activities once enjoyed.
- Neglecting personal hygiene or health: A noticeable decline in self-care.
- Problems at work or school: Decreased performance, frequent absences, or loss of employment/academic standing.
- Using substances to cope: Regularly turning to drugs or alcohol to deal with stress, sadness, anxiety, or trauma.
- Ineffective single-condition treatment: If someone has been treated for a mental health condition or a substance use disorder alone, but continues to struggle or relapse, it might indicate an untreated co-occurring condition.
Recognizing these signs is an important first step. If you or someone you care about is exhibiting these symptoms, it’s time to seek professional help. We encourage you to explore your options and Get Help Now. Our team at SoberSteps is ready to assist you in navigating the path to recovery.
Integrated Treatment: The Gold Standard for Recovery
When it comes to dual diagnosis, treating just one condition is like trying to row a boat with one oar – you’ll just go in circles. That’s why integrated treatment is considered the gold standard for recovery. This approach emphasizes treating both the mental health condition and the substance use disorder simultaneously, by the same team of professionals, or at least with highly coordinated care. The benefits of this integrated approach are profound: improved outcomes, reduced hospitalization rates, increased housing stability, and a significantly better quality of life for individuals. It’s about seeing the whole person, not just two separate problems.
Types of Treatment Approaches
Integrated treatment for dual diagnosis is comprehensive and often involves a combination of therapies and supports custom to the individual’s unique needs. There’s no one-size-fits-all solution, but a blend of evidence-based practices is typically most effective.
- Behavioral Health Support: This is a broad category encompassing various therapeutic interventions designed to help individuals manage their mental health and substance use. It’s about developing healthier coping mechanisms and life skills. Explore our Behavioral Health Support resources to learn more.
- Therapy: At the heart of dual diagnosis treatment is psychotherapy. Our Therapy page offers a deeper dive into different modalities. Some of the most effective include:
- Cognitive Behavioral Therapy (CBT): A widely used therapy that helps individuals identify and change negative thought patterns and behaviors contributing to their conditions. Find more about Cognitive Behavioral Therapy (CBT).
- Dialectical Behavior Therapy (DBT): Particularly effective for those with intense emotional dysregulation and a history of self-harm or suicidal ideation, DBT teaches skills in mindfulness, emotional regulation, distress tolerance, and interpersonal effectiveness. Learn more about Dialectical Behavior Therapy (DBT).
- Motivational Interviewing: This client-centered approach helps individuals explore and resolve their ambivalence about change, fostering intrinsic motivation for recovery. You can find more information on motivationalinterviewing.org.
- Medication-Assisted Treatment (MAT): For many, medications can play a crucial role in managing cravings, withdrawal symptoms, or mental health symptoms, especially for conditions like opioid use disorder, alcohol use disorder, depression, or anxiety. MAT, when combined with therapy, has shown to be highly effective.
- Support Groups: Peer support is invaluable. Groups like Alcoholics Anonymous (AA), Narcotics Anonymous (NA), and SMART Recovery provide a community where individuals can share experiences, gain insight, and receive encouragement.
- Individual Therapy: Provides a confidential space to address personal struggles, develop coping strategies, and work through underlying issues. Our Individual Therapy page has more details.
- Group Therapy: Offers a supportive environment where individuals can connect with others facing similar challenges, reduce feelings of isolation, and practice new skills in a safe setting. Explore the benefits of Group Therapy.
The “No Wrong Door” Policy
The “No Wrong Door” policy is a philosophy that has gained significant traction in the field of dual diagnosis treatment, championed by organizations like SAMHSA. It means that regardless of whether someone first seeks help for their mental illness or their substance use disorder, they should be screened for both and directed to integrated care. This policy aims to eliminate the historical silos between mental health and addiction services, ensuring that individuals don’t get turned away or bounced between systems because their primary presenting issue isn’t the “right” one for a particular facility.
SAMHSA’s promotion of this policy highlights its crucial role in effective treatment. By integrating screening and assessment, and ensuring that providers are equipped to address both conditions, we can significantly reduce barriers to care and improve treatment engagement and outcomes. It’s about creating a seamless, supportive system where every door leads to the right help.
Finding the Right Co-Occurring Disorders Treatment Program
Choosing the right treatment program is a critical step in the recovery journey. With so many options available, it can feel overwhelming, but knowing what to look for can simplify the process.
When searching for a program, we recommend prioritizing facilities that:
- Employ licensed professionals: Ensure the staff (therapists, doctors, counselors) are properly credentialed and experienced in treating both mental health and substance use disorders.
- Offer individualized treatment plans: No two people are alike, and effective treatment should be custom to your specific needs, challenges, and goals.
- Use evidence-based practices: Look for programs that rely on therapies and interventions proven effective through research, such as CBT, DBT, and MAT.
- Provide a continuum of care: Recovery is a journey, not a destination. The best programs offer support that extends beyond initial treatment, including aftercare planning, relapse prevention strategies, and connections to community resources.
We understand this can be a lot to consider. To help you steer your options, we invite you to explore our comprehensive guide on Co-occurring Disorders Treatment. It’s designed to answer your questions and connect you with reputable providers.
A Comprehensive Guide to Dual Diagnosis Resources
Navigating dual diagnosis resources can feel like searching for a needle in a haystack, especially when you’re already struggling. But rest assured, a wealth of support is available. This section is designed to be your toolkit, providing a clear roadmap to federal, national, and local support options. Reaching out is a sign of strength, and these resources are here to empower your journey to healing.
Federal and National Helplines
Sometimes, you need immediate support, a listening ear, or guidance on where to start. These helplines are confidential, often available 24/7, and are excellent first points of contact for anyone seeking dual diagnosis resources.
- SAMHSA National Helpline: This free, confidential, 24/7 information service, in English and Spanish, provides referrals to local treatment facilities, support groups, and community-based organizations. You can Call 1-800-662-HELP (4357) at any time. It’s a fantastic starting point for finding general mental health and substance use services.
- 988 Suicide & Crisis Lifeline: If you or someone you know is in emotional distress or suicidal crisis, the 988 Suicide & Crisis Lifeline is available 24/7 across the United States. You can call or text 988 to connect with trained crisis counselors who can provide immediate support and connect you to local resources.
- NAMI HelpLine: The National Alliance on Mental Illness (NAMI) operates a HelpLine that provides information, resources, and support to people living with mental illness and their families. While not a crisis line, it offers valuable guidance during business hours.
For a broader understanding of how these services work and what to expect, check out our Anonymous Hotline Mental Health Guide.
Government and Non-Profit Dual Diagnosis Resources
Beyond helplines, several key government agencies and non-profit organizations are dedicated to providing information, research, and policy guidance on mental health and substance use disorders. They are invaluable sources of credible dual diagnosis resources.
- Substance Abuse and Mental Health Services Administration (SAMHSA): As the lead federal agency for improving the behavioral health of the nation, SAMHSA offers a treasure trove of information, publications, and program support. Their Co-Occurring Disorders Page is an essential read for understanding integrated treatment and finding services.
- National Institute of Mental Health (NIMH): The NIMH is the largest federal research agency focused on mental disorders. Their research helps us understand the causes, treatments, and prevention of mental illnesses. Their NIMH page on Substance Use and Mental Health provides evidence-based insights into the complex relationship between these conditions.
- National Institute on Drug Abuse (NIDA): NIDA is the leading federal agency for scientific research on drug abuse and addiction. They provide crucial information on the science of addiction, including its impact on mental health. Explore their NIDA page on Co-Occurring Disorders for research-backed information.
- Mental Health America (MHA): MHA is a leading community-based non-profit dedicated to promoting mental health, preventing mental illness, and ensuring access to care. They offer screening tools, advocacy, and educational materials that can be highly beneficial.
Finding Local Treatment and Support
While national resources are excellent starting points, finding local, accessible treatment and support is often the most practical next step.
- SAMHSA’s Treatment Locator: This online tool is perhaps one of the most powerful dual diagnosis resources for finding local help. The SAMHSA’s Treatment Locator allows you to search for mental health and substance use treatment facilities by location, type of service, and payment options. It’s a comprehensive database that we highly recommend.
- Primary care provider referrals: Don’t underestimate the power of your family doctor. They can often provide referrals to local mental health professionals, therapists, or addiction specialists, and help coordinate your care.
- Mental Health Clinic options: Local clinics often provide a range of services, including therapy, medication management, and sometimes even integrated programs for dual diagnosis. Our guide to finding a Mental Health Clinic can help you explore options in your area.
- Understanding your insurance: Financial concerns can be a major barrier to treatment. Familiarizing yourself with your health insurance coverage for mental health and substance abuse services is crucial. Our Mental Health Insurance Complete Guide can help you steer this complex topic.
- Peer support groups: These groups offer a welcoming, non-judgmental environment where individuals can share their experiences and support each other. They are often free or low-cost and can be found in most communities:
- Alcoholics Anonymous (AA): For individuals seeking recovery from alcohol addiction.
- Narcotics Anonymous (NA): For individuals seeking recovery from drug addiction.
- SMART Recovery: A science-based program that helps individuals gain independence from addictive behaviors.
Finding the right support is a journey, and we are here to help every step of the way. Don’t hesitate to use these dual diagnosis resources to build your path to recovery.
The Circle of Support: Family, Friends, and Research
Recovery from dual diagnosis is rarely a solo endeavor. It thrives within a strong circle of support, which includes not only professional help but also the invaluable contributions of family, friends, and the continuous advancements in scientific research. These elements create a robust ecosystem that sustains long-term healing and well-being.
How Family and Friends Can Help
The role of loved ones in the recovery process cannot be overstated. Family and friends can be powerful allies, but it requires understanding, patience, and setting healthy boundaries.
- Educate yourself: Learning about dual diagnosis, its complexities, and the nature of addiction and mental illness is paramount. Understanding what your loved one is going through helps you respond with empathy rather than judgment.
- Encourage professional help: While you can offer support, professional treatment is essential. Gently encourage your loved one to seek and engage with integrated care, and offer to help them find appropriate dual diagnosis resources.
- Offer support without enabling: This is a delicate balance. Support means listening, being present, and showing love. Enabling means inadvertently making it easier for the person to continue their substance use or avoid responsibility for their mental health.
- Practice self-care: Supporting someone with a dual diagnosis can be emotionally draining. It’s crucial for family and friends to take care of their own mental and physical health. Support groups for families, like Al-Anon or Nar-Anon, can be incredibly helpful.
- Set healthy boundaries: Establishing clear boundaries is vital for both your well-being and your loved one’s recovery. This means defining what you can and cannot do, and sticking to those limits.
- Communication strategies: Learning to communicate effectively, actively listening, and expressing concerns without blame can strengthen relationships and foster a more supportive environment. SAMHSA offers valuable Resources for Families that can guide you through these challenging conversations.
The Role of Research and Clinical Trials
While we have effective treatments today, the field of dual diagnosis is constantly evolving thanks to ongoing research and clinical trials. These efforts are crucial for:
- Advancing understanding: Researchers continue to uncover the intricate biological, psychological, and social mechanisms underlying co-occurring disorders, leading to more targeted and effective interventions.
- Developing new treatments: Clinical trials test new medications, therapeutic approaches, and integrated care models, paving the way for innovative and improved treatment options.
- Improving outcomes: Through rigorous study, we learn which interventions are most effective for different individuals, allowing for more personalized and successful recovery journeys.
Clinical trials are research studies conducted with human volunteers to evaluate new ways to prevent, detect, or treat diseases. They are a critical step in bringing new treatments to patients. If you’re interested in contributing to scientific advancements or exploring cutting-edge treatments, you can often find current studies. For instance, you can search for ongoing clinical trials related to dual diagnosis on ClinicalTrials.gov. Participation is voluntary and carefully regulated to ensure patient safety.
Your Guide to Available Dual Diagnosis Resources
We want to reiterate that recovery from dual diagnosis is a journey, not a destination. It involves ups and downs, but with the right dual diagnosis resources and support, hope is real and achievable. Integrated treatment is the key to addressing both conditions effectively and fostering lasting wellness.
We’ve presented a wide array of dual diagnosis resources here, from national helplines and government agencies to local treatment programs and peer support groups. We encourage you to use these tools to take the first step, or the next step, in your or a loved one’s healing process. Don’t be afraid to ask for help; it’s the bravest thing you can do. Your journey to recovery is important, and there’s a whole community of support waiting for you.
Conclusion: Taking the Next Step Toward Healing
Navigating the complexities of co-occurring mental health and substance use disorders can feel overwhelming, but as we’ve explored, dual diagnosis is common and, most importantly, treatable. We’ve seen that integrated care, which addresses both conditions simultaneously, stands as the most effective approach to fostering lasting recovery and improving quality of life.
A wealth of dual diagnosis resources is available, ready to support you or your loved one on this journey. From federal helplines and national organizations like SAMHSA, NIMH, and NIDA, to local treatment centers and vital peer support groups, the pathways to healing are numerous and accessible. Remember the “No Wrong Door” policy, ensuring that help is available regardless of where you begin your search.
Recovery is not just a possibility; it’s a reality for millions. With the right support, custom treatment, and a robust network of care, you can achieve profound and sustainable healing.
At SoberSteps, we are an independent platform dedicated to helping individuals and families explore treatment and recovery options. We provide clear, actionable information and connect you with reputable providers. If you or a loved one is struggling with a dual diagnosis, please don’t face it alone. Take the first step today by exploring our comprehensive Co-occurring Disorders Treatment guide, or by calling our confidential 24/7 helpline to connect with paid advertiser treatment providers who can offer the specialized care you need. Your journey toward healing and a healthier future starts now.




