
Need Help Now? Your Immediate Guide to Addiction Support
Crisis? Get help now for suicide & addiction. Call 988 or SoberSteps for immediate, confidential support and treatment referrals. You’re not alone.

Unlock vital Medicaid Coverage for Addiction Treatment. Learn eligibility, covered services, and how to get help. Start recovery now!
Medicaid Coverage for Addiction Treatment is available to millions of Americans who need help with substance use disorders. Here’s what you need to know:
Addiction is a chronic disease that changes the brain and affects decision-making. Yet for too many people, the biggest barrier to recovery isn’t lack of motivation—it’s money. The cost of treatment can feel overwhelming when you’re already struggling.
That’s where Medicaid becomes a lifeline.
Medicaid is the single largest payer of behavioral health services in the United States, accounting for 30% of total spending on these services. In recent years, many Americans have grown to view substance use disorders as chronic diseases requiring medical treatment. This shift in understanding, combined with expanded coverage under the Affordable Care Act, has made quality addiction treatment more accessible than ever before.
Approximately 21% of Americans covered by Medicaid have a diagnosed substance use disorder—that’s millions of people who can access the care they need. For Medicaid recipients with alcohol use disorder, healthcare costs were on average 30% lower for those who received treatment medications compared to those who didn’t. Every dollar spent on methadone treatment generates $4 to $5 in healthcare savings.
If you or a loved one needs help, Get Help Now or call our Confidential Addiction Helpline. Recovery is possible, and you don’t have to figure this out alone.
At Sober Steps, we’ve helped thousands of individuals and families steer the complexities of Medicaid Coverage for Addiction Treatment and connect with quality care providers. Our team understands both the medical and financial aspects of recovery, and we’re here to guide you every step of the way.
Learn more about how SoberSteps can help you start recovery.
Medicaid is a cornerstone of the American healthcare system, providing vital health coverage to millions of low-income individuals and families. Its role in addressing substance use disorders has become increasingly critical, especially with the rising awareness that addiction is a treatable chronic disease. Understanding what Medicaid is and who it serves is the first step in open uping its potential for addiction treatment.
Medicaid is a joint federal and state government program that provides health coverage to millions of low-income Americans. While federal guidelines set some standards, each state administers its own Medicaid program, leading to variations in eligibility and covered services. This means that while the core purpose remains the same across the U.S., the specifics can differ significantly depending on where you live.
It’s a crucial safety net, ensuring that vulnerable populations, including children, pregnant women, the elderly, and people with disabilities, have access to necessary medical care. The Children’s Health Insurance Program (CHIP) is often discussed alongside Medicaid, as it provides low-cost health coverage to children in families who earn too much to qualify for Medicaid but cannot afford private insurance.
For official information and to understand the federal framework, you can always visit the official Medicaid information website.
Learn more about insurance and addiction treatment. When you’re ready, you can verify your insurance coverage with SoberSteps to see how your Medicaid plan can help.
Medicaid eligibility is primarily income-based, but it also considers other factors like family size, age, pregnancy status, and disability. Historically, eligibility was limited to specific “categorically needy” groups. However, the landscape shifted dramatically with the Affordable Care Act (ACA).
Key eligibility criteria generally include:
These are general guidelines. To find out if you qualify, we recommend checking your state’s specific eligibility requirements. You can also visit Medicaid.gov’s eligibility page for more information.
Don’t let uncertainty about eligibility keep you from seeking help. Check your eligibility and get help with SoberSteps today.
The Affordable Care Act (ACA), often called “Obamacare,” brought monumental changes to the healthcare landscape, profoundly impacting Medicaid Coverage for Addiction Treatment. Before the ACA, many low-income adults were left without health insurance, particularly if they weren’t pregnant, elderly, or disabled.
The ACA addressed this in two major ways:
This legislative shift has been a game-changer. As one statistic highlights, 21% of Americans covered by Medicaid have a diagnosed substance use disorder. The ACA’s provisions ensure that for this significant population, access to care is not just a hope, but a right. You can read more about the studies on the effects of Medicaid expansion and its positive impact.
To understand how these changes might specifically affect your access to care, we encourage you to explore how the ACA changed addiction treatment access. You can also find out how the ACA affects your coverage by reaching out to our team.
When we talk about Medicaid Coverage for Addiction Treatment, we’re not just referring to a single service. We’re talking about a broad spectrum of care designed to address every stage of a substance use disorder, from initial detox to long-term recovery support. This comprehensive approach is vital because addiction is a complex condition that requires individualized and ongoing care.
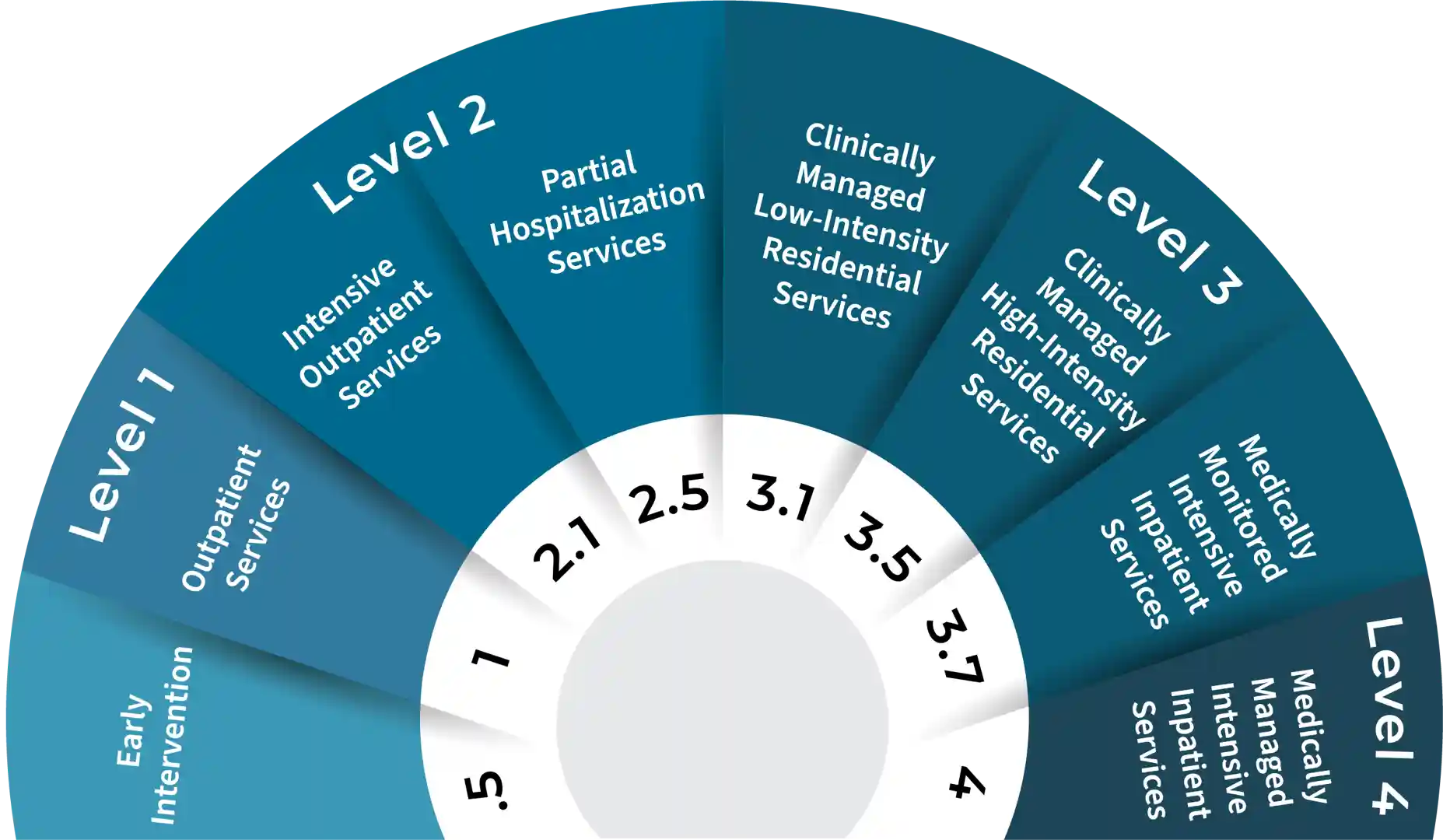
Medicaid is designed to cover a wide array of evidence-based addiction treatment services, ensuring that individuals can access the care they need at various stages of their recovery journey. While specific offerings can vary by state and individual plan, here’s a general list of services typically covered:
We encourage you to explore all levels of care available. To understand what your specific plan covers, you can see which services you can access with Medicaid.
While federal mandates and the ACA have significantly standardized certain aspects of Medicaid Coverage for Addiction Treatment, it’s crucial to remember that Medicaid is a state-administered program. This means there can be noticeable differences in how coverage is implemented from one state to another. These variations can impact:
For a deeper dive into how states manage and deliver behavioral health care, we recommend reviewing reports like How states deliver behavioral health care.
This variability means that what’s covered in one state might not be exactly the same in another. It’s why we always recommend verifying your specific state’s Medicaid benefits. Ready to take the next step? Find a Medicaid-accepting rehab near you. We also have a dedicated resource to help you learn about state-specific Medicaid coverage.
The opioid crisis has devastated communities across the United States, and Medicaid has emerged as an indispensable tool in the fight against it. Its expansive reach among low-income populations, who are often disproportionately affected by substance use disorders, makes it a primary payer for crucial interventions.
Medicaid’s role in addressing the opioid crisis includes:
Medicaid is not just a payment mechanism; it’s a critical component of the American substance use disorder prevention, intervention, and treatment infrastructure, especially in the context of the ongoing opioid epidemic.
If you or someone you know is struggling with opioid addiction, please don’t wait. We can help you explore opioid addiction treatment options. Get help for opioid addiction now and start your journey to recovery.
Navigating healthcare, especially for something as sensitive as addiction treatment, can feel daunting. But with Medicaid Coverage for Addiction Treatment, you have a powerful resource. We’re here to break down the practical steps to help you use your benefits and find the right treatment center.
Finding a facility that accepts your specific Medicaid plan is a crucial step. While 71% of drug and alcohol treatment facilities in the United States accepted Medicaid in 2020, knowing where to look can save you time and stress. Here’s how we recommend you proceed:
Don’t let the search overwhelm you. Call our confidential helpline for assistance. We’re here to simplify the process and help you find a Medicaid-accepting rehab that’s right for you.
Within the field of Medicaid, particularly in states that use Managed Care Organizations (MCOs), you might encounter different types of plans, most commonly Health Maintenance Organizations (HMOs) and Preferred Provider Organizations (PPOs). Understanding the differences between these can help you make an informed choice about your care.
| Feature | Medicaid HMO (Health Maintenance Organization) | Medicaid PPO (Preferred Provider Organization) |
|---|---|---|
| Provider Network | Typically smaller, more restricted network of doctors and facilities. | Larger network of “preferred” providers; some coverage for out-of-network. |
| Primary Care Physician (PCP) | Usually required to choose a PCP who coordinates all your care. | Not typically required to choose a PCP. |
| Referrals | Generally requires a referral from your PCP to see specialists or receive treatment. | Usually no referral needed to see specialists within the network. |
| Flexibility | Less flexibility in choosing providers; must stay in-network for most coverage. | More flexibility in choosing providers; can see out-of-network for higher cost. |
| Costs | Often lower premiums and out-of-pocket costs (if any). | Potentially higher out-of-pocket costs for out-of-network services. |
| Addiction Treatment Access | Must use in-network facilities and follow referral processes. | Can choose from a wider range of facilities, including some out-of-network. |
For addiction treatment, the implications of choosing an HMO or PPO can be significant. An HMO might mean fewer choices for specialized rehab centers, but potentially fewer out-of-pocket expenses. A PPO offers more freedom to choose a specific facility or therapist, but you’ll need to be mindful of network status to avoid unexpected costs.
We’re here to help you sort through these details. Learning how to choose the right insurance plan for rehab is important. Don’t hesitate to get help choosing your Medicaid plan or understanding its benefits.
One of the greatest advantages of Medicaid Coverage for Addiction Treatment is its affordability. For many beneficiaries, the costs associated with treatment are significantly reduced or even eliminated entirely. However, it’s still important to be aware of potential costs and limitations:
Understanding these aspects is key to effectively utilizing your benefits. We encourage you to learn how to pay for addiction treatment and to get help understanding your Medicaid benefits. Our team is here to clarify any confusion and guide you toward the care you deserve.
When discussing public health insurance and addiction treatment, it’s common for questions to arise about the differences between Medicaid and Medicare. While both are government programs, they serve distinct populations and have different structures. We’ll also explore what happens when someone qualifies for both and the crucial role of parity laws.
While both Medicaid and Medicare are government-funded health insurance programs, they are designed for different populations and have unique coverage structures for addiction treatment.
Medicaid:
Medicare:
The key takeaway is that Medicaid focuses on income-based need, while Medicare focuses on age or long-term disability. For a detailed look at how these programs interact with other payers, refer to how Medicaid interacts with other payers.
To understand your options better, especially if you’re approaching Medicare eligibility, we have resources that explain Medicare and addiction treatment explained. If you’re wondering about coverage, learn about your options if you have Medicare and Medicaid.
It’s entirely possible for an individual to qualify for both Medicaid and Medicare—this is known as being “dual eligible.” These individuals often have complex healthcare needs and limited incomes, making the combined benefits of both programs incredibly valuable for accessing comprehensive care, including addiction treatment.
Here’s how dual eligibility typically works:
For individuals seeking Medicaid Coverage for Addiction Treatment, being dual eligible offers significant advantages:
If you believe you might be eligible for both programs, it’s worth exploring. This combined coverage can be a powerful tool in supporting your recovery journey without the burden of high costs.
We’re here to help you steer this complex area. Learn about dual diagnosis treatment if you have co-occurring conditions. For specific questions, get help with dual eligibility questions.
The Mental Health Parity and Addiction Equity Act (MHPAEA) is a landmark federal law enacted in 2008 that has fundamentally reshaped how insurance plans, including Medicaid, cover mental health and substance use disorder (SUD) treatment. Its core principle is simple but profound: benefits for mental health and SUDs should be no more restrictive than those for medical and surgical benefits.
What does this mean in practice for Medicaid Coverage for Addiction Treatment?
MHPAEA has been a critical policy tool, helping to dismantle discriminatory practices and creating a more equitable landscape for individuals seeking help for addiction. It reinforces the understanding that addiction is a health condition deserving of comprehensive care, just like any other physical illness.
For official guidance and detailed information on parity laws, you can visit Medicaid.gov’s official information on Parity. Understanding your rights under these laws is crucial, and we encourage you to learn about mental health parity and your rights. If you have questions, understand your rights under parity laws by reaching out to our team.
We understand that navigating Medicaid Coverage for Addiction Treatment can bring up many questions. Here, we address some of the most common inquiries we receive to help you feel more confident about your options.
Yes, you can still get addiction treatment with Medicaid even if your state did not expand its program under the Affordable Care Act (ACA). However, your eligibility will be based on traditional Medicaid categories, which are often more restrictive.
In non-expansion states, Medicaid typically covers:
If your state hasn’t expanded Medicaid, and you don’t fall into one of these traditional categories, your options for Medicaid coverage may be limited. However, other resources, such as state-funded programs or grants, might be available.
It’s always best to check your state’s specific eligibility rules, as they can change. You can also check your eligibility now through our service, or explore our state-by-state Medicaid eligibility guide.
Generally, Medicaid covers addiction treatment services at facilities that are enrolled as Medicaid providers. These facilities must meet specific state and federal requirements for care quality and cost-effectiveness.
While the quality of care at Medicaid-accepting facilities can be excellent and evidence-based, they are typically not what would be considered “luxury” or high-end private rehab centers. These types of facilities often cater to individuals with private insurance or those who can pay out-of-pocket, and their higher operating costs usually mean they do not accept Medicaid reimbursement rates.
Medicaid’s focus is on providing medically necessary, effective, and accessible treatment options. This means you can expect comprehensive care, including medical detox, therapy, counseling, and medication-assisted treatment, but usually within a standard clinical environment rather than one offering premium amenities.
To get a better understanding of what to expect, we recommend you read what to expect from Medicaid-covered rehab. You can also find out what Medicaid-covered rehab is like by speaking with our team.
Receiving a denial for your Medicaid application can be disheartening, but it’s not necessarily the end of the road. You have rights, and there are steps you can take:
The appeals process exists for a reason, and many denials are overturned. Don’t give up on seeking the coverage you need for addiction treatment.
We understand this can be a stressful time. If you need support, you can contact SoberSteps for help with your application. We also have resources on how to appeal a Medicaid denial to guide you.
Medicaid Coverage for Addiction Treatment plays an absolutely vital role in the health and well-being of millions of Americans. It has transformed access to care, particularly for low-income individuals and families who were historically underserved. Thanks to the Affordable Care Act (ACA) and the Mental Health Parity and Addiction Equity Act (MHPAEA), addiction treatment is increasingly recognized and covered as essential healthcare, just like any other medical condition.
Recovery from a substance use disorder is not only possible but also more affordable than ever before, thanks to these critical programs. We’ve seen how Medicaid covers a comprehensive range of services, from detox and residential care to outpatient therapy and life-saving medications, demonstrating its commitment to a full continuum of care. Moreover, the economic benefits of treating addiction through Medicaid—such as significant healthcare savings—underscore its value to both individuals and society.
Don’t let the perceived cost or complexity be a barrier to seeking the help you or a loved one deserves. The journey to recovery is challenging enough; financial worry shouldn’t add to that burden.
If you or a loved one are struggling and need help navigating your options, SoberSteps offers a Confidential Addiction Helpline to connect you with treatment providers who understand your needs and insurance options.
Start your recovery journey today. We’re here to support you every step of the way.
Contact SoberSteps for personalized support.

Crisis? Get help now for suicide & addiction. Call 988 or SoberSteps for immediate, confidential support and treatment referrals. You’re not alone.

Decode your mental health insurance. Explore coverage, laws, plan types, and steps to access care. Get empowered to use your benefits.

Why a Recovery Support System is Essential for Lasting Sobriety A Recovery support system is your network of people and resources that help you maintain sobriety.
For anyone seeking help for addiction for themselves or a loved one calls to Sober Steps are completely confidential and available 24/7.
Please note: any treatment center listed on our site that receives calls is a paid advertiser.
Calls to a specific treatment center’s listing will be connected directly to that center.
Calls to our general helpline will be answered by treatment providers, all of whom are paid advertisers.
By calling the helpline, you agree to our terms and conditions. These calls are free of charge and carry no obligation to enter treatment. Neither Sober Steps nor anyone answering your call receives a commission or fee based on your choice of treatment provider.
If you’d like to explore additional treatment options or connect with a specific rehab center, you can browse our top-rated listings, visit our homepage, or call us at (844) 491-5566. You may also contact us for further assistance.