
Why Medicaid Coverage for Addiction Treatment Matters
Medicaid Coverage for Addiction Treatment is a lifeline available to millions of Americans. Here’s what you need to know:
- Yes, Medicaid covers addiction treatment – including detox, inpatient rehab, outpatient programs, medications, and counseling
- Eligibility is primarily income-based – typically for those earning below 138% of the Federal Poverty Level in expansion states
- Coverage varies by state – but the Affordable Care Act requires essential substance use disorder services
- Most treatment facilities accept it – 71% of drug and alcohol treatment facilities accepted Medicaid in 2020
- Costs are usually low or zero – most states don’t require co-payments for addiction treatment
Addiction is a chronic disease, but for many, the biggest barrier to recovery isn’t motivation—it’s the overwhelming cost of treatment. That’s where Medicaid becomes essential.
As the single largest payer for behavioral health services in the U.S., Medicaid has become crucial. A growing understanding of addiction as a treatable disease, combined with the Affordable Care Act, has made quality treatment more accessible. About 21% of Medicaid recipients have a substance use disorder, giving millions access to care. Treatment is also cost-effective: healthcare costs are 30% lower for those with alcohol use disorder who get treatment, and every dollar spent on methadone saves $4 to $5.
If you or a loved one needs help, Get Help Now or call our Confidential Addiction Helpline. Recovery is possible.
At Sober Steps, we’ve helped thousands steer Medicaid Coverage for Addiction Treatment and connect with quality care providers. Our team is here to guide you every step of the way.
Learn more about how SoberSteps can help you start recovery.
Understanding Medicaid and Its Role in Addiction Care
Medicaid is a cornerstone of the American healthcare system, providing vital health coverage to millions of low-income individuals and families. Its role in addressing substance use disorders has become increasingly critical. Understanding what Medicaid is and who it serves is the first step in accessing its potential for addiction treatment.

What is Medicaid?
Medicaid is a joint federal-state program providing health coverage to low-income Americans. While the federal government sets standards, each state runs its own program, so eligibility and services vary. It’s a crucial safety net for children, pregnant women, the elderly, and people with disabilities. The Children’s Health Insurance Program (CHIP) is a related program for children. For official details, visit the official Medicaid information website. When you’re ready, verify your insurance coverage with SoberSteps to see how your plan can help.
Who is Eligible for Medicaid?
Medicaid eligibility is mainly based on income relative to the Federal Poverty Level (FPL), but also considers family size, age, and disability. The Affordable Care Act (ACA) significantly expanded who qualifies.
Key groups include:
- Income-based: Households below a state-specific FPL percentage.
- Pregnant women & Children: Often qualify at higher income levels.
- Adults in expansion states: Typically adults with incomes up to 138% of the FPL.
- Individuals with disabilities: Those on Supplemental Security Income (SSI) often automatically qualify.
To confirm if you qualify, check your state’s rules or visit Medicaid.gov’s eligibility page. Don’t let uncertainty stop you. Check your eligibility and get help with SoberSteps today.
How the Affordable Care Act (ACA) Expanded Access
The Affordable Care Act (ACA) profoundly impacted Medicaid Coverage for Addiction Treatment. Before the ACA, many low-income adults had no insurance options. The ACA changed this in two key ways:
- Medicaid Expansion: It allowed states to cover nearly all adults with incomes up to 138% of the Federal Poverty Level. This has been critical for closing care gaps for addiction treatment in the 41 states (plus DC) that adopted it.
- Essential Health Benefits (EHBs): The ACA required all new insurance plans, including Medicaid, to cover a set of EHBs. Crucially, this includes mental health and substance use disorder services, which must be covered at parity with medical care.
These changes have been a game-changer, ensuring the 21% of Medicaid recipients with a substance use disorder have a right to care. You can read more about the studies on the effects of Medicaid expansion. To see how these changes affect you, find out how the ACA affects your coverage by reaching out to our team.
Comprehensive Medicaid Coverage for Addiction Treatment
Medicaid Coverage for Addiction Treatment includes a broad spectrum of care designed to address every stage of a substance use disorder. This comprehensive approach is vital because addiction is a complex condition that requires ongoing, individualized care.

What Specific Addiction Treatment Services Does Medicaid Cover?
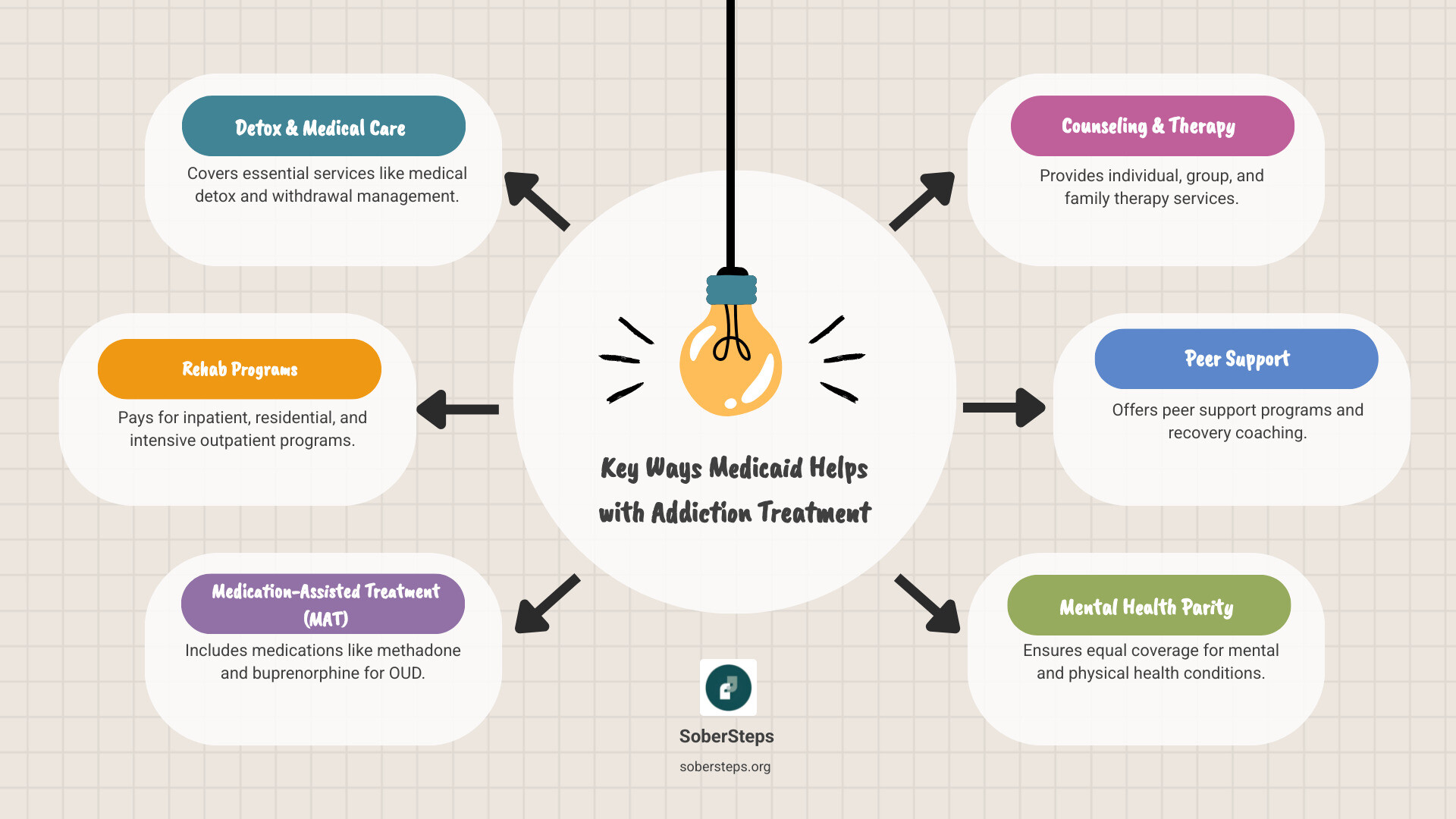
Medicaid covers a wide range of evidence-based services for every stage of recovery. While specifics vary by state, coverage typically includes:
- Medical Detoxification (Detox): Medically supervised withdrawal management. Learn more about Levels of Care: Detox.
- Inpatient/Residential Treatment: 24/7 care in a structured, live-in setting. Explore Levels of Care: Inpatient.
- Intensive Outpatient (IOP) & Partial Hospitalization (PHP): Structured treatment while living at home. Discover Levels of Care: Intensive Outpatient.
- Medication-Assisted Treatment (MAT): Combines FDA-approved medications with therapy for opioid and alcohol use disorders.
- Counseling and Therapy: Individual, group, and family therapy, including Cognitive Behavioral Therapy.
- Peer Support Services: Guidance from individuals with lived recovery experience.
- Aftercare and Continuing Care: Ongoing support like sober living and relapse prevention. Consider Levels of Care: Aftercare.
We encourage you to explore all levels of care. To see what your specific plan covers, see which services you can access with Medicaid.
State-by-State Differences in Medicaid Coverage for Addiction Treatment
Because Medicaid is state-administered, Medicaid Coverage for Addiction Treatment varies. Key differences include:
- Eligibility Thresholds: Income limits differ, especially between expansion and non-expansion states.
- Covered Services: States have flexibility in the scope and duration of services.
- Managed Care Organizations (MCOs): Private plans contracted by the state may have different provider networks and rules.
- Provider Networks: The number of facilities accepting Medicaid can vary by state.
For a deeper dive, review reports on how states deliver behavioral health care. This variability makes it essential to check your state’s specific benefits. Ready to take the next step? Find a Medicaid-accepting rehab near you.
Medicaid’s Critical Role in the Opioid Crisis
Medicaid is an indispensable tool in fighting the opioid crisis, especially for low-income populations. Its role includes:
- Comprehensive MAT Coverage: As the gold standard for opioid use disorder (OUD), Medicaid is a major funder of Medication-Assisted Treatment (MAT).
- Access to Naloxone: All states cover this life-saving overdose reversal medication. You can learn more about Medicaid access to Naloxone policies.
- Cost-Effectiveness: Treatment is a smart investment. Every $1 spent on methadone saves $4 to $5 in healthcare costs.
- Support for Vulnerable Populations: Medicaid provides a treatment pathway for individuals who might otherwise have no access.
If you or someone you know is struggling with opioid addiction, we can help you explore opioid addiction treatment options. Get help for opioid addiction now and start your recovery.
How to Use Your Medicaid Benefits for Rehab
Navigating healthcare for addiction treatment can feel daunting. With Medicaid Coverage for Addiction Treatment, you have a powerful resource. Here are the practical steps to use your benefits and find the right care.
Finding Treatment Centers That Accept Medicaid
While 71% of treatment facilities accepted Medicaid in 2020, finding one in your plan is the first step. Here’s how to start:
- SAMHSA’s FindTreatment.gov: Use this confidential federal directory to search for facilities by location and payment option, including Medicaid.
- Your State Medicaid Agency: Your state’s official Medicaid website has provider directories and contact information.
- Your Medicaid Plan: If you have a Managed Care plan, call the number on your card for a list of in-network providers.
- Reach Out to SoberSteps: Our team specializes in connecting people with providers that accept their insurance. We can also help you find free rehab centers near you.
Don’t let the search overwhelm you. Call our confidential helpline for assistance. We’re here to simplify the process and help you find a Medicaid-accepting rehab that’s right for you.
Understanding Medicaid Plans: HMO vs. PPO
In states with Managed Care Organizations (MCOs), you may encounter HMO or PPO plans. Understanding the difference is key.
| Feature | Medicaid HMO (Health Maintenance Organization) | Medicaid PPO (Preferred Provider Organization) |
|---|---|---|
| Provider Network | Smaller, restricted network. Must stay in-network. | Larger network; some out-of-network coverage. |
| Referrals | Usually requires a referral from a Primary Care Physician (PCP). | Referrals not typically required for in-network specialists. |
| Flexibility | Less flexibility in choosing providers. | More flexibility to choose providers. |
| Costs | Often lower or no out-of-pocket costs. | May have higher costs for out-of-network care. |
An HMO may limit your choice of rehab centers but keep costs down. A PPO offers more freedom but requires you to watch network status to avoid unexpected bills. We can help you choose the right insurance plan for rehab. Get help choosing your Medicaid plan or understanding its benefits.
Potential Costs and Limitations
A major benefit of Medicaid Coverage for Addiction Treatment is its affordability, but it’s wise to know about potential limitations:
- Co-payments: Most states have very low or no co-pays for addiction treatment.
- Prior Authorization: Intensive services like inpatient rehab may require pre-approval from your plan to be covered.
- Network Restrictions: You must use providers in your plan’s network to ensure coverage.
- Waitlists: High demand can sometimes lead to waitlists for certain treatment types.
- The IMD Exclusion: A historical rule limited funding for larger residential facilities, but recent changes and state waivers have greatly expanded access to this type of care.
Understanding these aspects is key. We can help you learn how to pay for addiction treatment and get help understanding your Medicaid benefits.
Medicaid, Medicare, and Other Key Factors
When discussing public health insurance, questions often arise about Medicaid and Medicare. While both are government programs, they serve distinct populations. We’ll also explore what happens when someone qualifies for both and the crucial role of parity laws.
Medicaid vs. Medicare for Addiction Treatment
While both are government-funded, Medicaid and Medicare serve different groups and cover addiction treatment differently.
Medicaid:
- Eligibility: For low-income individuals and families.
- Costs: Very low or no out-of-pocket costs.
- Coverage: Comprehensive, covering a full continuum of care.
Medicare:
- Eligibility: For people 65+ or those with certain long-term disabilities.
- Costs: Involves premiums, deductibles, and co-insurance.
- Coverage: Split into parts: Part A (inpatient), Part B (outpatient), and Part D (prescriptions).
In short, Medicaid is based on income, while Medicare is based on age or disability. For more details, refer to how Medicaid interacts with other payers. If you have questions about your options, learn about your options if you have Medicare and Medicaid.
Dual Eligibility: Using Both Medicaid and Medicare
Some people qualify for both Medicaid and Medicare—this is known as being “dual eligible.” This is highly beneficial for those with complex health needs and limited incomes.
Here’s how it works:
- Medicare Pays First: Medicare is the primary payer for covered services.
- Medicaid Pays Second: Medicaid then covers costs Medicare doesn’t, like deductibles and co-payments.
For addiction treatment, dual eligibility means lower out-of-pocket costs and broader coverage. This is particularly helpful for those with co-occurring mental health disorders. For example, individuals with co-occurring conditions like PTSD can find help for co-occurring disorders like PTSD. Get help with dual eligibility questions from our team.
The Role of the Mental Health Parity and Addiction Equity Act (MHPAEA)
The Mental Health Parity and Addiction Equity Act (MHPAEA) is a landmark law ensuring that insurance benefits for mental health and SUDs are no more restrictive than those for medical care.
For Medicaid Coverage for Addiction Treatment, this means:
- Equal Treatment: Plans cannot impose stricter financial requirements or treatment limitations on SUD benefits than on medical/surgical benefits.
- Impact on Medicaid: The law applies to Medicaid Managed Care Organizations (MCOs), ensuring equitable coverage for most beneficiaries.
- Increased Access: MHPAEA has been shown to increase the number of SUD treatment facilities that accept Medicaid.
This law reinforces that addiction is a health condition deserving the same level of care as any physical illness. For official details, visit Medicaid.gov’s official information on Parity. Understand your rights under parity laws by reaching out to our team.
Frequently Asked Questions about Medicaid and Addiction Treatment
We understand that navigating Medicaid Coverage for Addiction Treatment can bring up many questions. Here, we address some of the most common inquiries.
Can I get addiction treatment with Medicaid if my state didn’t expand it?
Yes, but eligibility is more limited. In non-expansion states, Medicaid is generally restricted to traditional categories like low-income pregnant women, children, and individuals who are elderly or have a qualifying disability. Other state-funded programs might be available. It’s always best to check your state’s specific rules. You can check your eligibility now or explore our state-by-state Medicaid eligibility guide.
Does Medicaid cover private or luxury rehab facilities?
Generally, no. Medicaid covers treatment at facilities enrolled as Medicaid providers, which must meet standards for cost-effective, evidence-based care. While the quality of care is often excellent, these are not luxury centers. Medicaid’s focus is on providing medically necessary and accessible treatment in a standard clinical setting. To learn more, find out what Medicaid-covered rehab is like by speaking with our team.
What should I do if my application for Medicaid is denied?
A denial isn’t the final word. You have the right to appeal.
- Understand the Reason: Your denial notice will explain why you were rejected.
- Gather Documents: Collect any information that can support your case.
- File an Appeal: Follow the instructions on the denial notice to file an appeal before the deadline.
- Seek Assistance: You don’t have to do this alone. Legal aid services or patient advocates can offer guidance.
Many denials are overturned on appeal. If you need support, contact SoberSteps for help with your application. We also have resources on how to appeal a Medicaid denial.
Conclusion
Medicaid Coverage for Addiction Treatment is a vital lifeline. It has made recovery possible and affordable for millions by expanding access to care. Thanks to laws like the Affordable Care Act (ACA) and the Mental Health Parity and Addiction Equity Act (MHPAEA), addiction treatment is covered as the essential healthcare it is.
Recovery from a substance use disorder is possible and more affordable than ever. Medicaid covers a full continuum of care, from detox to therapy. Don’t let cost or complexity stop you or a loved one from getting help.
If you need help navigating your options, SoberSteps offers a Confidential Addiction Helpline to connect you with treatment providers who understand your needs and insurance options.
Start your recovery journey today. We’re here to support you every step of the way.



